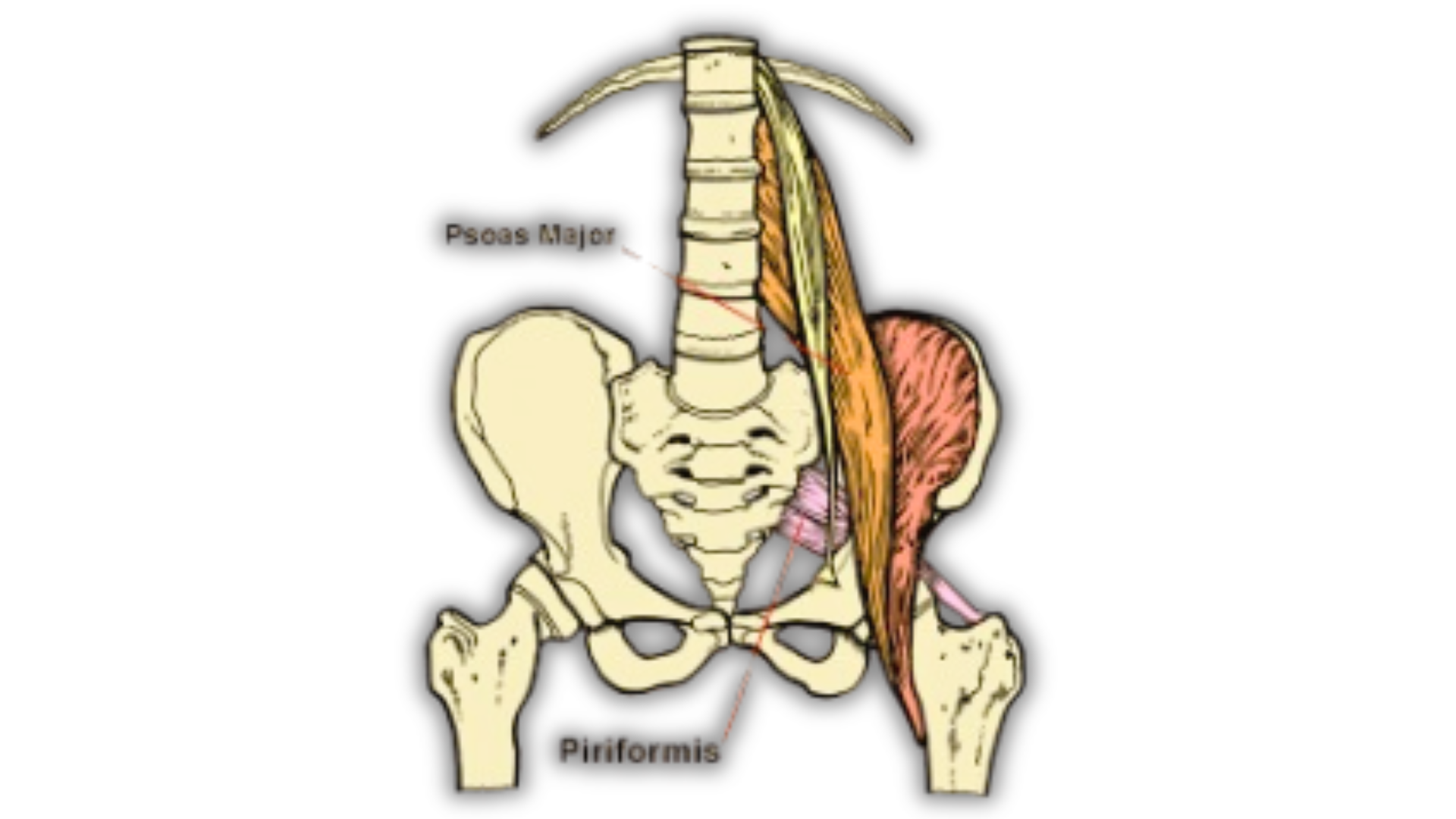
Have you ever felt tightness in your hip, lower back, or deep in your buttocks that just doesn’t seem to go away? Many people feel this kind of discomfort, and sometimes it’s linked to two muscles called the psoas and the piriformis. When these muscles become tight or out of balance, they can cause stiffness, which is called psoas–piriformis syndrome. It isn’t a medical diagnosis, but it’s an easy way to describe what’s going on.
ANF Therapy® is an advanced option that supports your body’s healing mechanisms to relieve muscle tightness. A trained practitioner places small ANF Devices on the skin in areas of tension. In this blog, we’ll talk about what it is, why it happens, and how ANF Therapy® may help you.
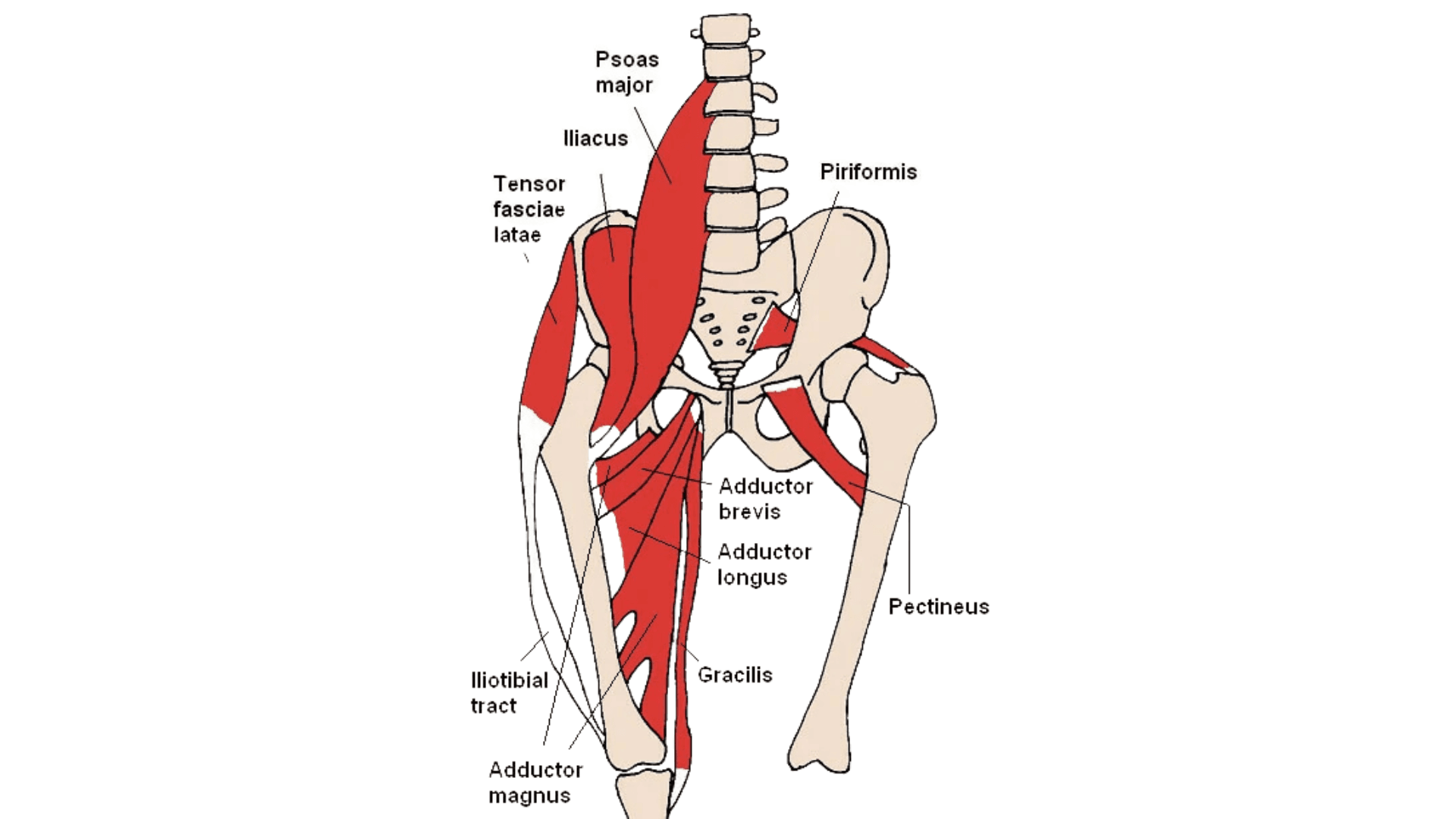
What Are the Psoas and Piriformis Muscles?
Psoas:
The psoas major is one of the deepest muscles in the body. It originates along the lumbar spine and inserts into the femur. Because of its location, it plays a major role in:
- Hip flexion (lifting the leg)
- Stabilizing the spine
- Supporting the pelvis during movement
- Helping with posture and gait mechanics
The psoas is often called a “fight-or-flight” muscle because it tends to tighten under chronic stress, long hours of sitting, or repetitive hip-flexion activities such as running or cycling.
Piriformis:
The piriformis is a small triangular muscle located deep in the buttocks, running from the sacrum to the top of the femur. Its main roles include:
- Help rotate the hip externally
- Stabilizing the sacrum and pelvis
- Controlling leg and hip alignment during walking
The piriformis is located close to the sciatic nerve, which is why irritation or tightness in this muscle can sometimes contribute to nerve-related symptoms.

What Is Psoas–Piriformis Syndrome?
Psoas–piriformis syndrome is a combined pattern of tightness, tension, or overactivity in both the psoas and piriformis muscles. Instead of functioning independently, these muscles influence one another through the pelvis and spine. When one muscle becomes tight or irritated, the other often compensates, creating a cycle of imbalance.
Common contributing factors include:
The following factors can contribute to psoas-piriformis syndrome.
- Prolonged sitting
- Stress-related muscle tension
- Overuse from sports
- Weakness in the surrounding core or hip muscles
- Postural habits that tilt the pelvis
- Previous injury in the hip, pelvis, or lower back
This combination of factors may lead to discomfort or restricted movement in various areas, not only the hip or buttock, but also the spine and pelvis.
Common symptoms of psoas-piriformis syndrome
Because the psoas and piriformis affect both the spine and hips, symptoms can vary widely. Many people describe a mixture of:
1. Deep hip or buttock tightness
A feeling of deep gripping or tightness, especially after long periods of sitting or standing.
2. Lower-back discomfort
The psoas attaches directly to the lumbar spine, so tension in the muscle may be felt in the lower back.
3. Pelvic imbalance or stiffness
Some individuals feel like one side of the pelvis is “higher,” “twisted,” or less mobile.
4. Radiation downward
Because the piriformis lies near the sciatic nerve, tightness in that area can sometimes contribute to leg discomfort or tingling.
5. Difficulty with hip rotation
Activities like crossing the legs, squatting, or pivoting the hips may feel limited or uncomfortable.
These symptoms may appear gradually or suddenly, depending on the underlying cause.
Why are these two muscles becoming a team problem?
When the psoas tightens, it can tilt the pelvis forward (anterior pelvic tilt), increasing strain on the lower back. The piriformis often responds by tightening to stabilize the pelvis. In other cases, the piriformis becomes irritated first, such as after a fall, an intense workout, or repetitive rotation, and the psoas tightens secondarily to compensate for the instability. This is why both muscles often require attention, even if only one seems problematic.
How to manage psoas-piriformis syndrome?
Various therapies help manage the psoas Piriformis syndrome. These include:
1-ANF Therapy®:
ANF Therapy® is an innovative approach that aids standard treatment in the management of musculoskeletal problems such as the psoas-piriformis syndrome. This therapy utilises small ANF Devices that are applied to the affected areas of your body to support healing naturally.
Outcomes:
A real-world study involved 1,054 patients across 45 countries to assess the effectiveness of ANF Therapy®. Common pain areas included the lower back, knee, neck, and shoulder. As a result, pain levels decreased significantly, from 7.6 to 3.1 out of 10 with ANF Therapy®. Patients also showed reduced swelling and improved range of motion. Satisfaction was high (92/100), and side effects, such as dry mouth, headache, and fatigue, were mild and short-term, reported by 42% of patients. These results show that ANF Therapy® is helpful in supporting the recovery of orthopaedic injuries.
Start your journey with ANF Therapy®:
ANF Therapy® is the newest frequency-based approach. If you have psoas–piriformis syndrome, consult an ANF Practitioner or find an ANF Therapist at www.anftherapy.com/find-clinic/ to discuss how ANF Therapy® can help.
If you’re a healthcare practitioner and want to enhance your clinical skills with frequency medicine, learn more about the ANF Therapy® and ANF Clinical education program by visiting www.anfacademy.com
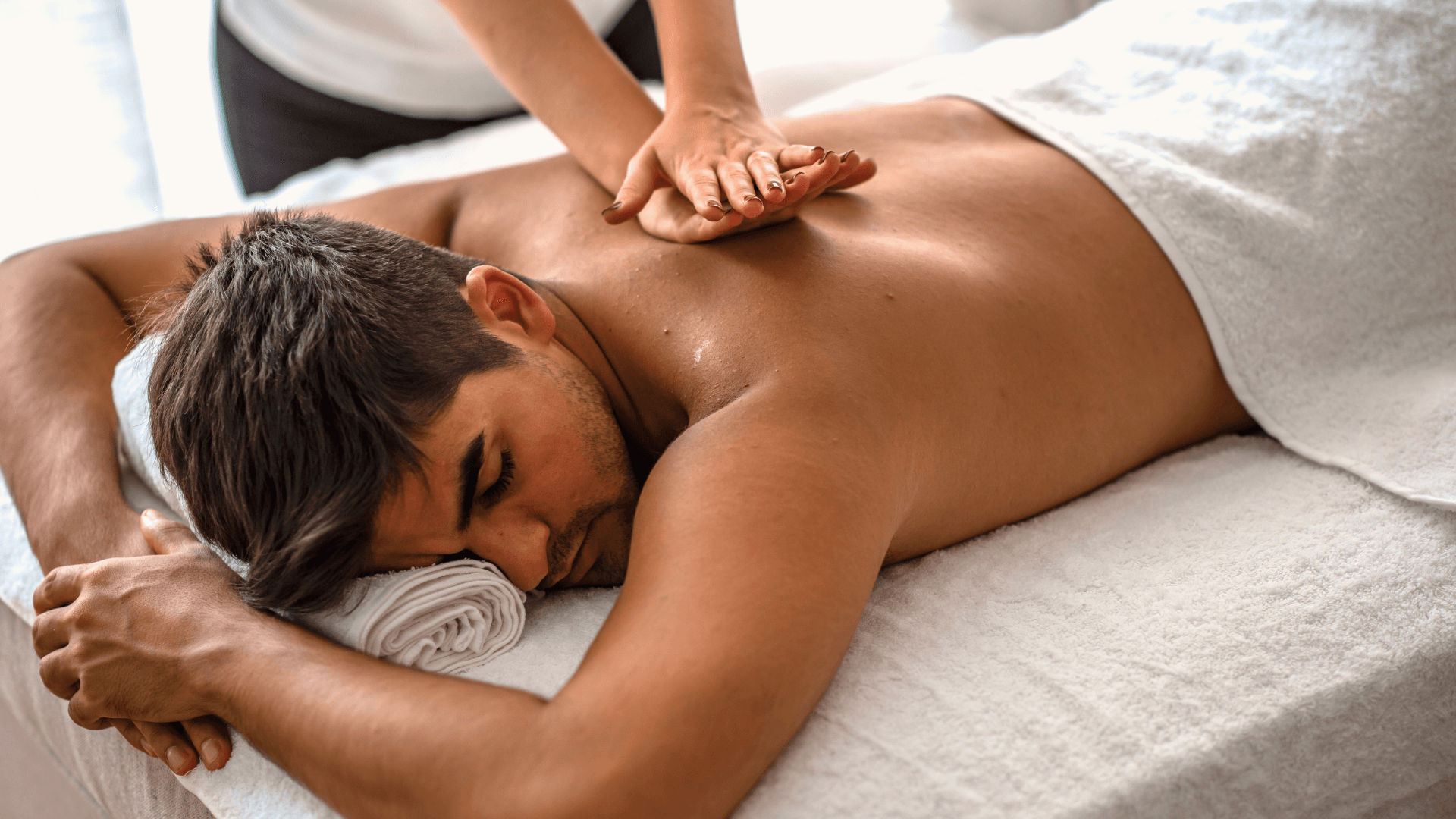
2-Manual therapy and soft-tissue techniques
Some therapists may use the following:
- Myofascial release
- Trigger-point work
- Deep-tissue massage
- Stretch-assisted therapy
These methods can help ease tightness in the psoas, piriformis, glutes, and surrounding hip muscles. Some therapists also work on adjacent structures like the quadratus lumborum, hip flexors, or sacroiliac region to address contributing tension.
3. Stretching
Gentle stretching is often used to improve mobility and reduce excessive tightness. Common stretches include:
- Psoas stretch (half-kneeling hip-flexor stretch)
- Piriformis stretch (figure-four stretch)
- Supine knee-to-chest stretch
- Gentle spinal rotation stretches
The key is slow, controlled movement, avoiding any forcing or aggressive pushing into discomfort.
4. Strengthening exercise
Strengthening the core and hips can help support the pelvis and reduce compensatory load on the psoas and piriformis. These include the following areas.
- Deep core muscles (transverse abdominis)
- Glute muscles (gluteus medius, gluteus maximus)
- Lower abdominal muscles
- Hip stabilizers
Exercises may include bridges, clamshells, modified planks, or hip-abduction work, depending on the individual’s needs.

5. Postural and movement training
Therapists often look at how a person sits, walks, stands, or exercises. Minor adjustments such as modifying chair height, altering running form, or changing lifting mechanics can help reduce unnecessary strain on the psoas and piriformis.
6. Heat, relaxation, and breathing work
Because the psoas is closely linked to the body’s stress response, relaxation techniques can be helpful. Some approaches include:
- Heat therapy
- Diaphragmatic breathing
- Gentle yoga-based mobility
- Mindfulness practices
These techniques may help reduce nervous-system-driven tension in deep hip and core muscles.
7. Activity
When symptoms begin to improve, a gradual return to regular movement or exercise is often recommended. Jumping back into high-intensity workouts too quickly can re-irritate the area, so pacing is important.
Conclusion
Psoas–piriformis syndrome is a helpful way to describe the pattern of tightness and imbalance that can develop between these two deep hip muscles. Approaches such as ANF Therapy®, stretching, strengthening, postural adjustments, and relaxation techniques may support better movement and help reduce discomfort. With consistent attention to the body’s needs, you can move with greater ease and maintain a more balanced foundation in the hips, spine, and pelvis.