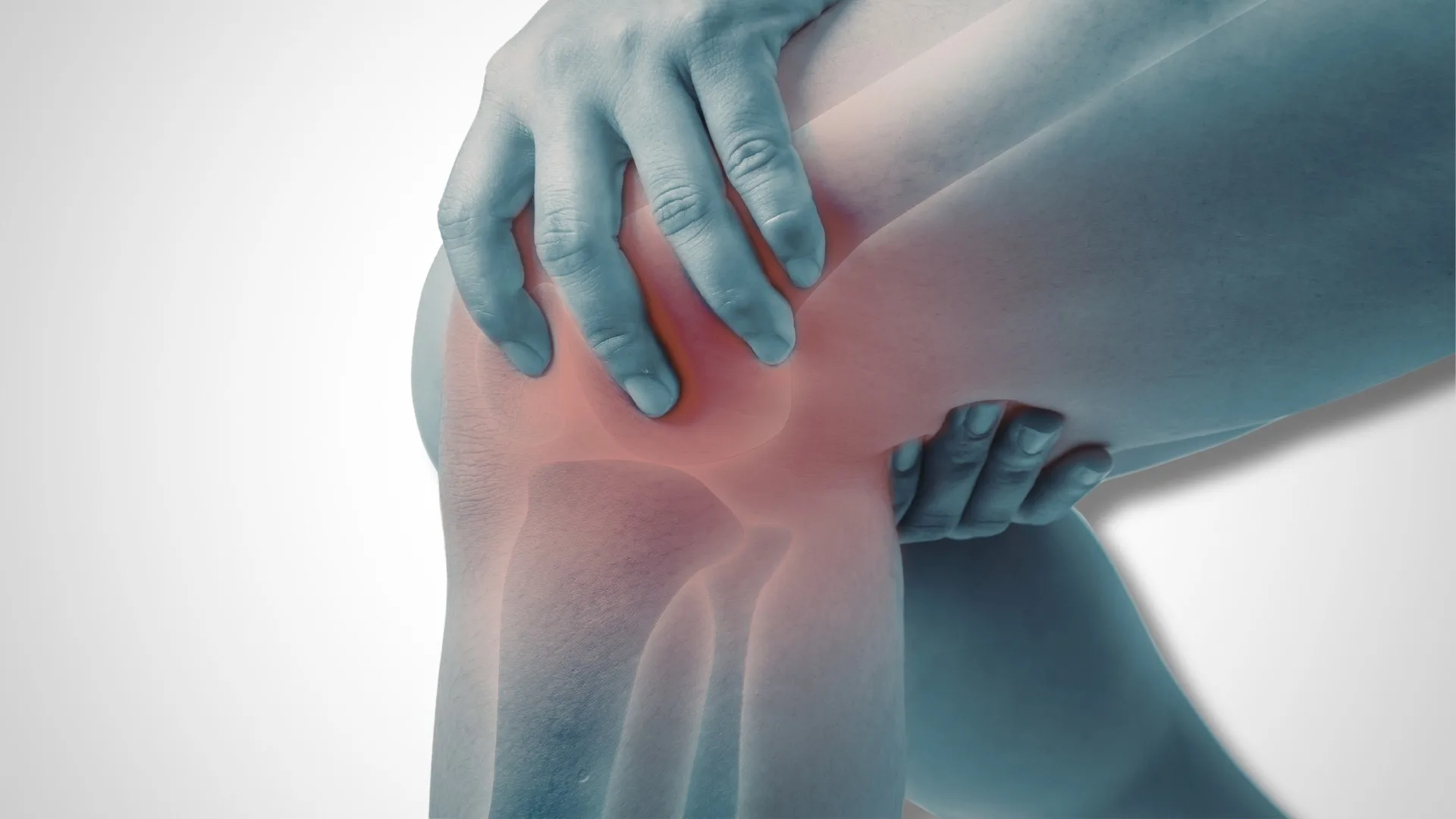
Why Does My Knee Snap on the Outside? Understanding Snapping Biceps Femoris Syndrome
It is a musculoskeletal condition that often affects athletes and physically active individuals, but some disorders remain relatively unknown despite causing significant discomfort. One such condition is Snapping Biceps Femoris Syndrome, a rare painful condition characterized by lateral knee pain and an audible snapping sensation during movement.
ANF Therapy® is an advanced approach that can be used as a supportive option alongside standard medical treatments to help manage this condition.
In this blog, we will discuss the anatomy involved, causes, symptoms, diagnosis, treatment options, and prevention strategies for Snapping Biceps Femoris Syndrome.
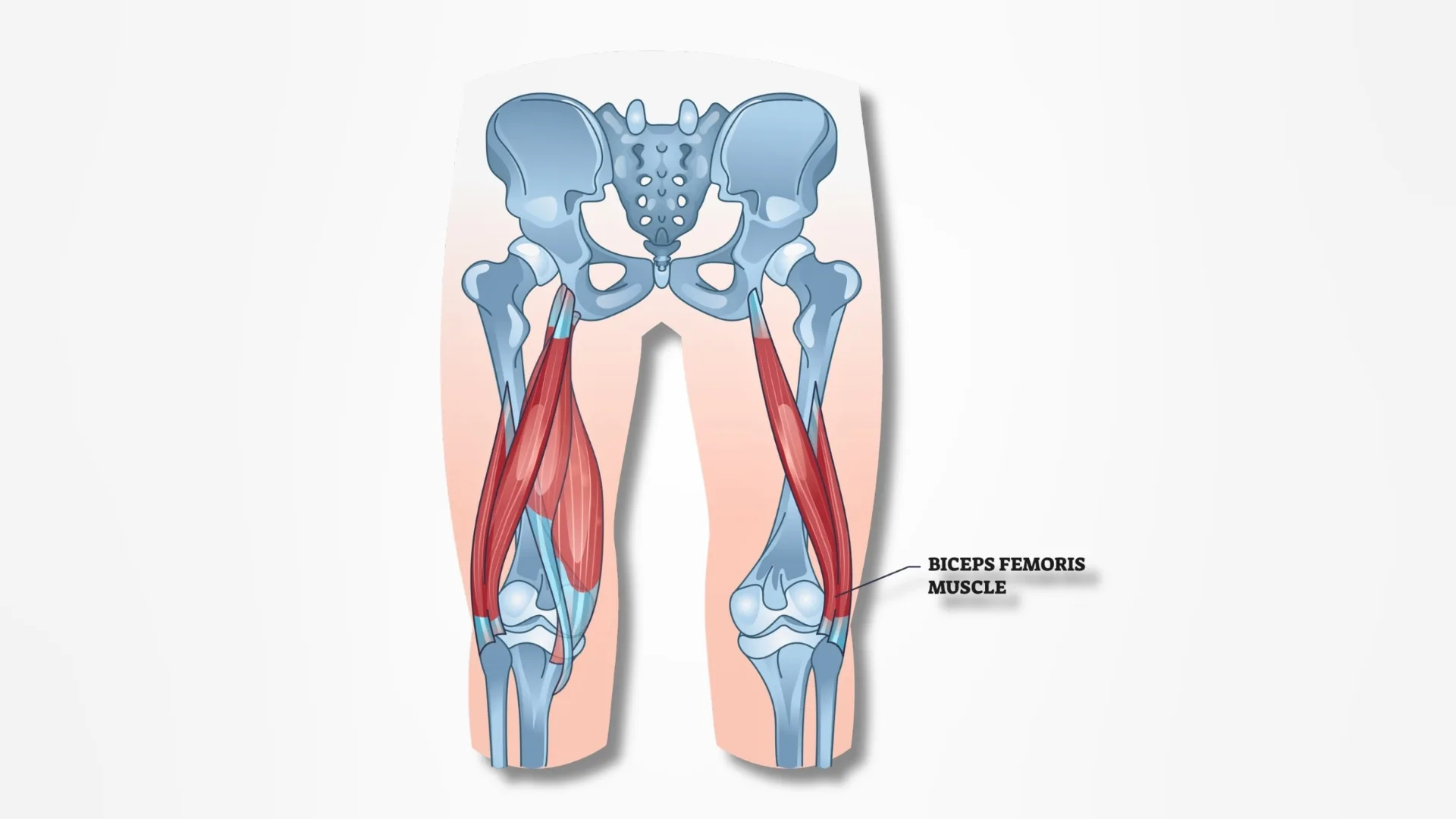
Understanding the Anatomy: The Biceps Femoris Muscle
It is important to understand the structure involved before discussing the syndrome. The biceps femoris is one of the three muscles that make up the hamstring group located at the back of the thigh. It plays a key role in bending the knee and extending the hip.
The biceps femoris has two heads:
- Long head: It originates from the ischial tuberosity of the pelvis.
- Short head: It originates from the femur.
Both heads merge into a tendon that inserts mainly into the head of the fibula, a small bone located on the outer side of the lower leg near the knee. This tendon helps stabilize the knee and assists in movements like running, jumping, and squatting.
In Snapping Biceps Femoris Syndrome, the tendon of this muscle abnormally moves or “snaps” over nearby bone structures, leading to a noticeable clicking or snapping sensation during movement.
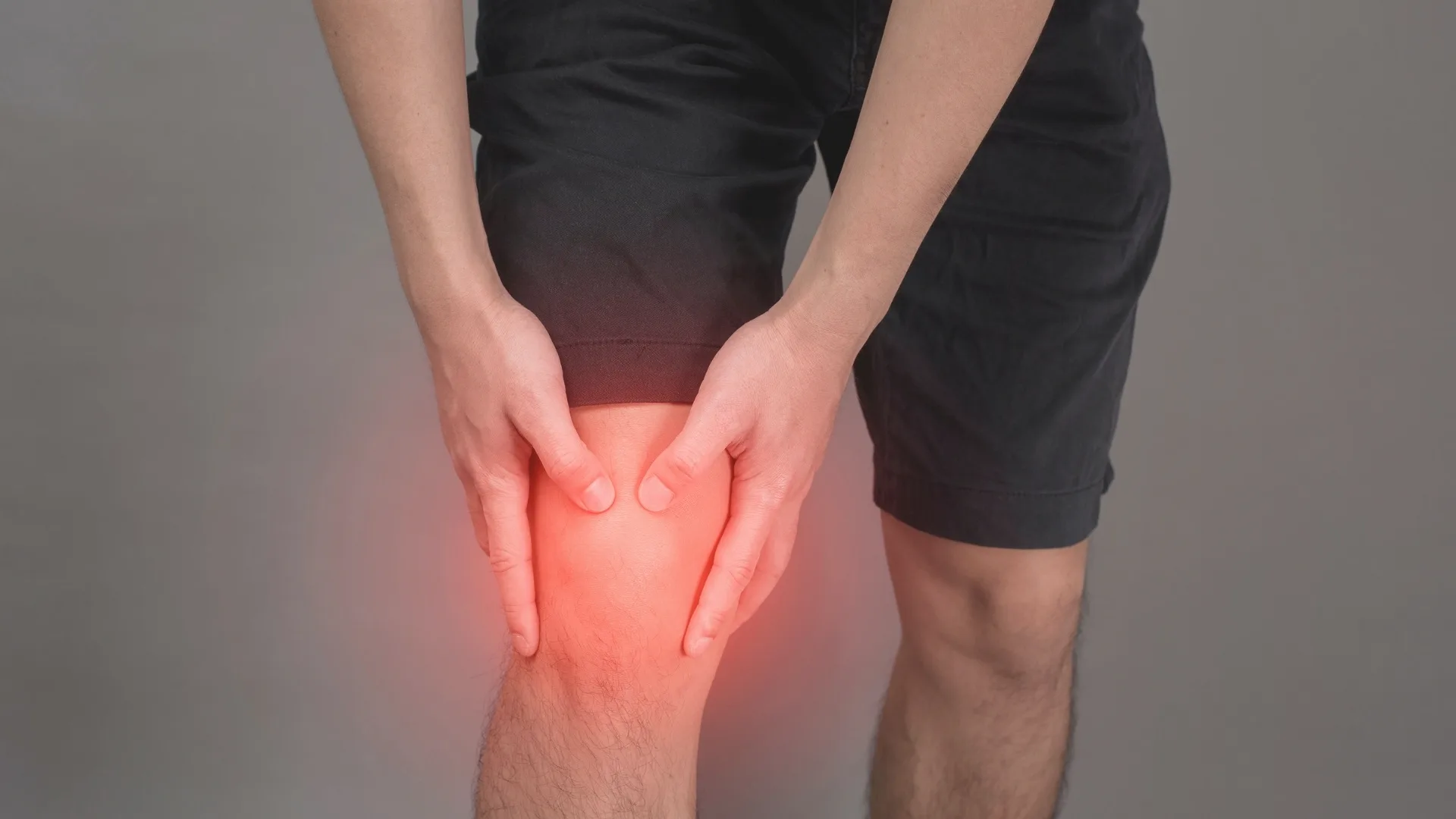
What Is Snapping Biceps Femoris Syndrome?
Snapping Biceps Femoris Syndrome is a rare orthopedic condition in which the distal tendon of the biceps femoris muscle moves over the fibular head or nearby structures, producing an audible snapping or popping sensation on the outer side of the knee.
This snapping typically occurs when the knee bends and straightens. While some snapping conditions in the body are painless, this syndrome often causes discomfort, irritation, and sometimes chronic knee pain.
The condition may occur due to abnormal tendon insertion, fibular head deformity, injury, or repetitive stress from physical activities.

Causes of Snapping Biceps Femoris Syndrome
Several factors can contribute to the development of this syndrome. In many cases, it results from structural abnormalities or overuse.
1. Anatomical Variations
Some individuals naturally have variations in how the biceps femoris tendon attaches to the fibula. These abnormal insertions may cause the tendon to move improperly during knee motion, leading to snapping.
2. Fibular Head Prominence
If the head of the fibula is unusually prominent or shaped differently, it can act like a mechanical obstacle, causing the tendon to slide or snap across it.

3. Trauma or Injury
Previous knee injuries, especially those affecting the posterolateral structures of the knee, can alter the alignment or tension of the tendon. Scar tissue formation may also contribute to snapping.
4. Repetitive Athletic Movements
Athletes involved in sports that require frequent knee flexion, such as soccer, sprinting, cycling, or weightlifting, may develop irritation or mechanical changes in the tendon over time.
5. Tight Hamstrings
Limited flexibility in the hamstring muscles can increase tension on the biceps femoris tendon, potentially contributing to abnormal movement.
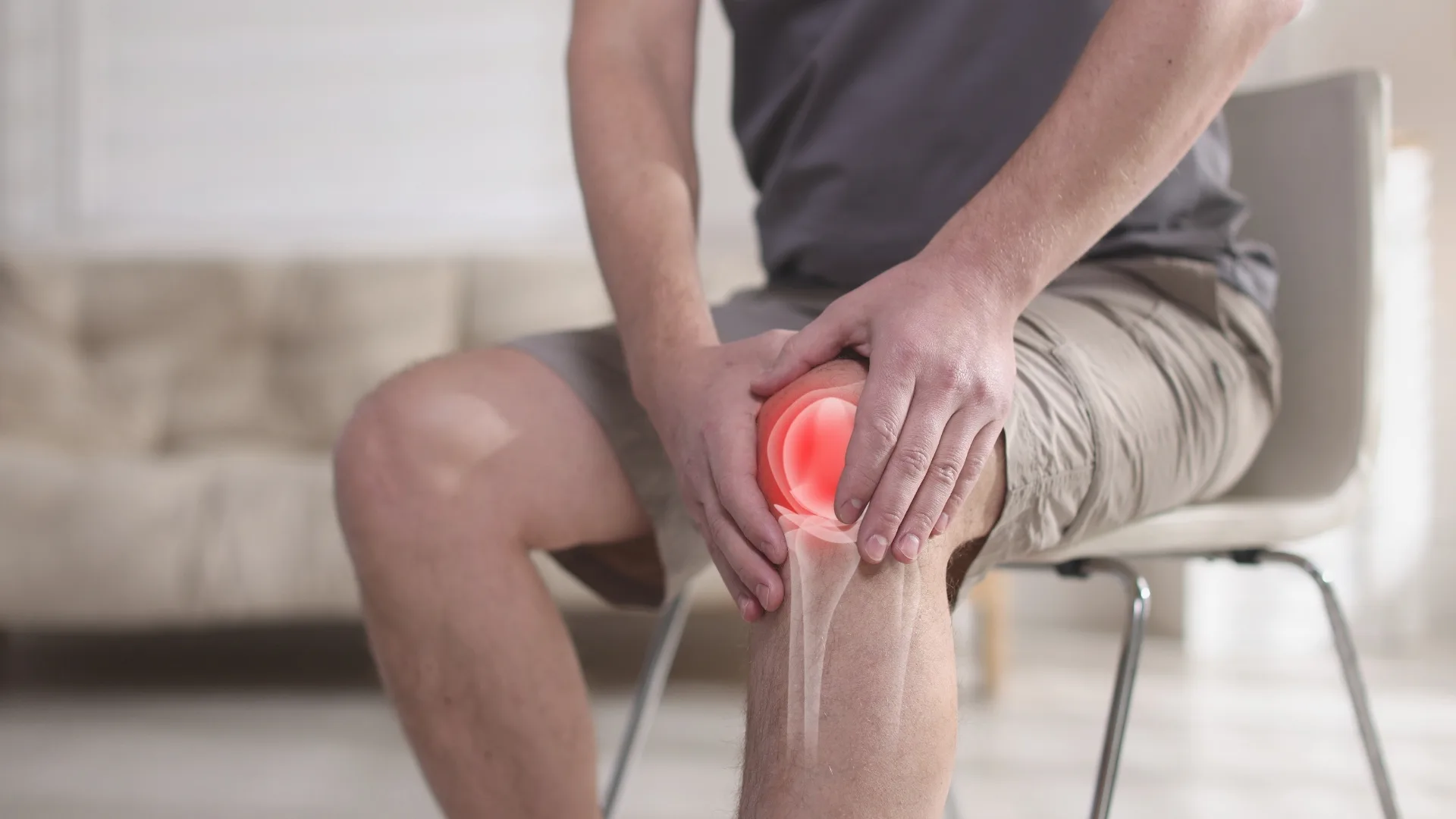
Common Symptoms
The hallmark feature of Snapping Biceps Femoris Syndrome is the audible or palpable snapping sensation on the outer side of the knee. However, symptoms can vary among individuals.
Typical symptoms include:
- Audible snapping or popping during knee bending
- A feeling of something “moving” over the outer knee
- Pain or discomfort on the lateral side of the knee
- Tenderness near the fibular head
- Swelling in some cases
- Reduced athletic performance
- Difficulty with deep squats or running
In some individuals, the snapping may be painless initially but becomes painful over time due to inflammation.

Who Is at Risk?
Although the condition is rare, certain groups are more susceptible.
High-risk individuals include:
- Athletes (especially runners and soccer players)
- Weightlifters performing heavy squats
- Individuals with previous knee injuries
- People with congenital tendon insertion variations
- Those with poor hamstring flexibility
Treatment Options
Treatment depends on the severity of symptoms and how much the condition affects daily activities.
Conservative (Non-Surgical) Treatment
Nowadays, many patients prefer non-surgical treatment options rather than relying on medications or invasive procedures. As a result, most cases are initially managed with conservative treatment approaches that focus on reducing pain, improving function, and promoting natural healing.
ANF Therapy®
ANF Therapy® is an advanced, frequency-based, non-invasive approach that can be used alongside standard medical treatments to manage musculoskeletal issues. This therapy utilises small wearable ANF Devices that are applied to certain areas of your body. It supports the body’s natural healing processes and promotes overall wellness.
Outcomes
ANF Therapy® is a chemical-free modality. Its effectiveness has been observed and studied in real-world clinical settings. A study involving 1,054 patients across 45 countries evaluated the use of ANF Therapy® for various musculoskeletal concerns. Commonly addressed areas included the lower back, knees, neck, and shoulders. Reported pain scores decreased from an average of 7.6 to 3.1 out of 10 following ANF Therapy® use. Participants also reported reduced swelling and improved range of motion. Overall satisfaction scores were high, while reported effects such as dry mouth, headache, or fatigue were mild and short-term. These findings reflect how ANF Therapy® can be used in supportive care settings for musculoskeletal recovery and neuromuscular balance.
Start Your Journey With ANF Therapy®
ANF Therapy® is a frequency-based approach that supports the body’s natural processes. It is used as a complementary approach along with physiotherapy and medical treatment for individuals experiencing a wide range of musculoskeletal discomforts, such as snapping bicep femoris syndrome. If you are experiencing chronic knee pain and a snapping sound in your knee during movement, consult an ANF Practitioner to discuss whether ANF Therapy® could be included as part of your personal wellness or recovery strategy.
You can find an ANF Therapist by visiting: www.anftherapy.com/find-clinic.
If you are a healthcare professional interested in expanding your understanding of frequency-based approaches, you can check out more information about ANF Therapy® and the ANF Clinical Education Program at www.anfacademy.com.

Other conservative therapies include the following:
Rest and Activity Modification
It is important to take rest and avoid the activities that trigger the snapping. It helps reduce irritation and inflammation.
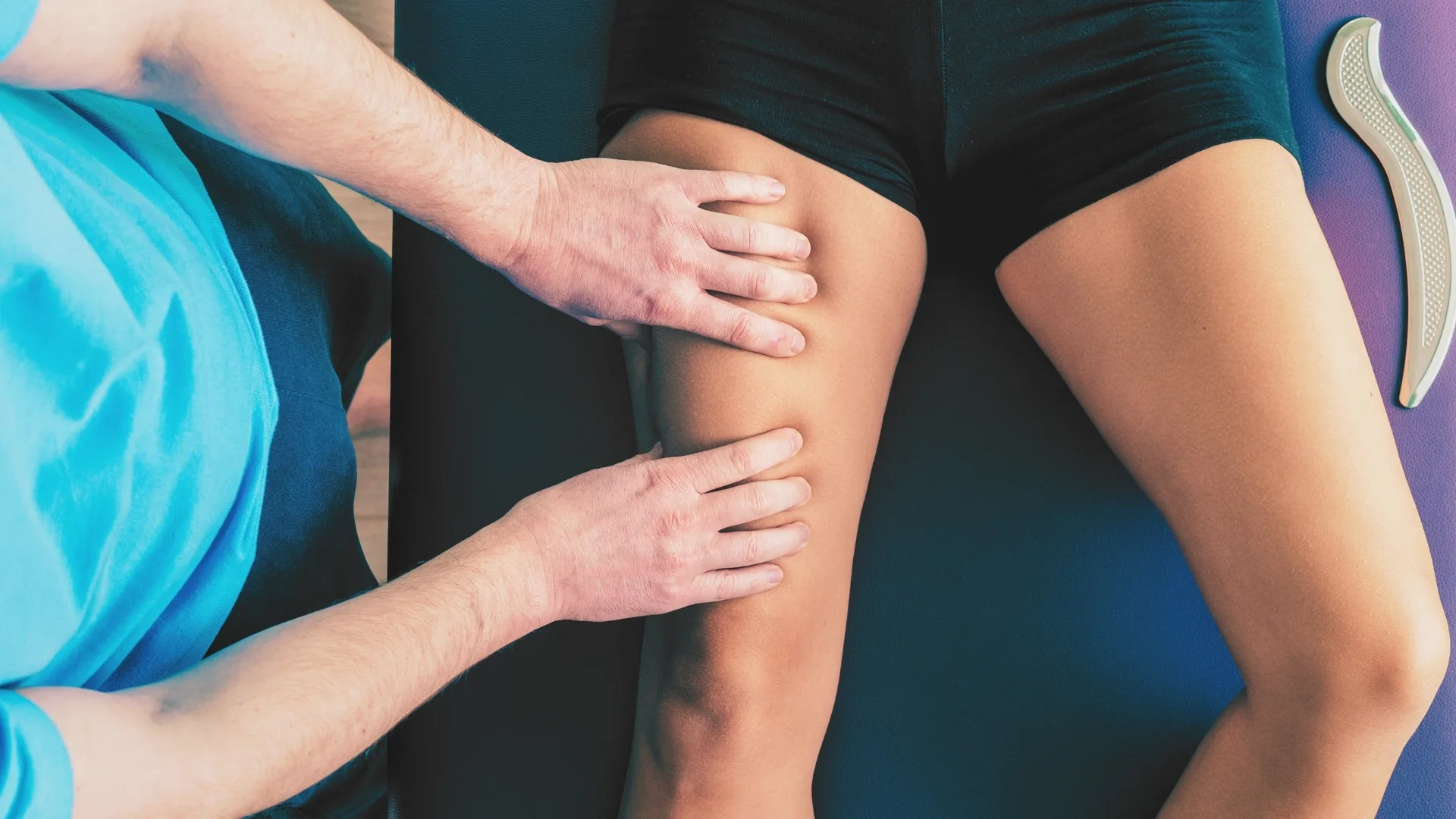
Physical Therapy
Physiotherapy plays a major role in treatment. Therapy typically focuses on:
- Hamstring stretching
- Strengthening surrounding muscles
- Improving knee stability
- Correcting movement patterns

Ice Therapy
Applying ice to the affected area after physical activity can help reduce swelling, inflammation, and discomfort associated with snapping biceps femoris syndrome. Cold therapy helps numb the area and limit inflammation, providing temporary pain relief. Individuals are usually advised to apply an ice pack to the outer side of the knee for about 15–20 minutes after activities that trigger symptoms.

Sports Technique Correction
Correcting sports techniques is an important part of conservative management, especially for athletes. Improper running, squatting, or lifting techniques can place extra stress on the hamstring muscles and the biceps femoris tendon. Biomechanical analysis by a physiotherapist can help identify these issues and guide athletes in adjusting their movement patterns to reduce tendon strain and prevent further irritation.

Prevention Strategies
While not every case can be prevented, there are several steps you can take to reduce your risk of developing snapping biceps femoris syndrome and protect your knee health.
Maintain Hamstring Flexibility
Make sure you regularly stretch your hamstrings. Keeping these muscles flexible helps reduce tension on the biceps femoris tendon and allows smoother knee movement during daily activities and sports.
Strengthen Supporting Muscles
Focus on strengthening the muscles that support your knee, including your glutes, quadriceps, and core. Strong supporting muscles improve knee stability and reduce excess strain on the hamstring tendons.
Warm Up Properly
Before any workout, training session, or sports activity, take time to perform a proper warm-up. Dynamic warm-up exercises prepare your muscles and joints for movement and help lower the risk of injury.
Avoid Sudden Training Increases
Try to increase your training intensity gradually. Sudden increases in exercise duration, speed, or load can put excessive stress on the tendon and increase the likelihood of irritation or injury.
Address Knee Pain Early
If you notice snapping, discomfort, or pain around the outer side of your knee, do not ignore it. Early evaluation by a physiotherapist or sports medicine specialist can help identify the problem and prevent it from worsening.
Conclusion
Snapping Biceps Femoris Syndrome is a rare condition that can cause snapping sensations and pain on the outer side of the knee, especially in athletes and physically active individuals. It occurs when the biceps femoris tendon moves abnormally over the fibular head during knee movement. Although the snapping may seem harmless at first, persistent symptoms should not be ignored.
In many cases, the condition can be managed effectively with conservative treatments such as rest, physiotherapy, movement correction, and supportive approaches like ANF Therapy®. Maintaining hamstring flexibility, strengthening supporting muscles, and addressing knee discomfort early can also help prevent the condition from worsening. Most individuals can return to normal activities and maintain healthy knee function with proper care and early management.