Proximal Hamstring Tendinopathy: A Complete Guide to Causes, Symptoms, and Recovery
Proximal hamstring tendinopathy (PHT) is a chronic overuse injury that affects your hamstring tendon where it attaches to the pelvis at the ischial tuberosity, commonly known as the “sitting bone.” Unlike an acute hamstring strain that happens suddenly during sprinting, proximal hamstring tendinopathy develops gradually over time due to repetitive stress and insufficient recovery.
This condition is particularly common in runners, cyclists, soccer players, and individuals who perform repetitive hip flexion activities. It can also affect people who sit for long hours, as sustained pressure on the hamstring origin may irritate the tendon.
ANF Therapy® is a frequency-based complementary approach used alongside standard medical treatment for the management of proximal hamstring tendinopathy. In this blog, we will discuss proximal hamstring tendinopathy, including what it is, why it develops, its symptoms, and how ANF Therapy® may help.
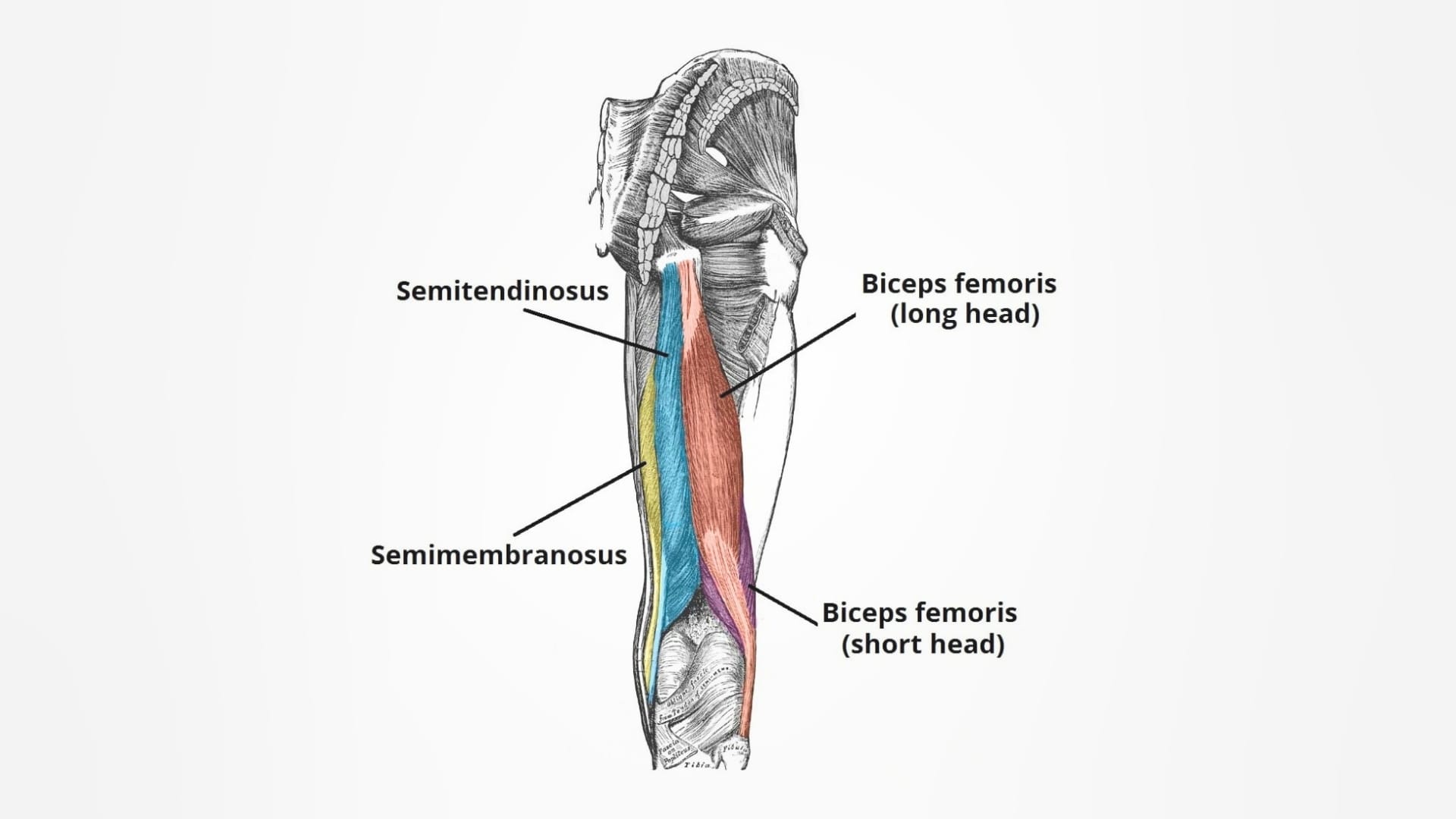
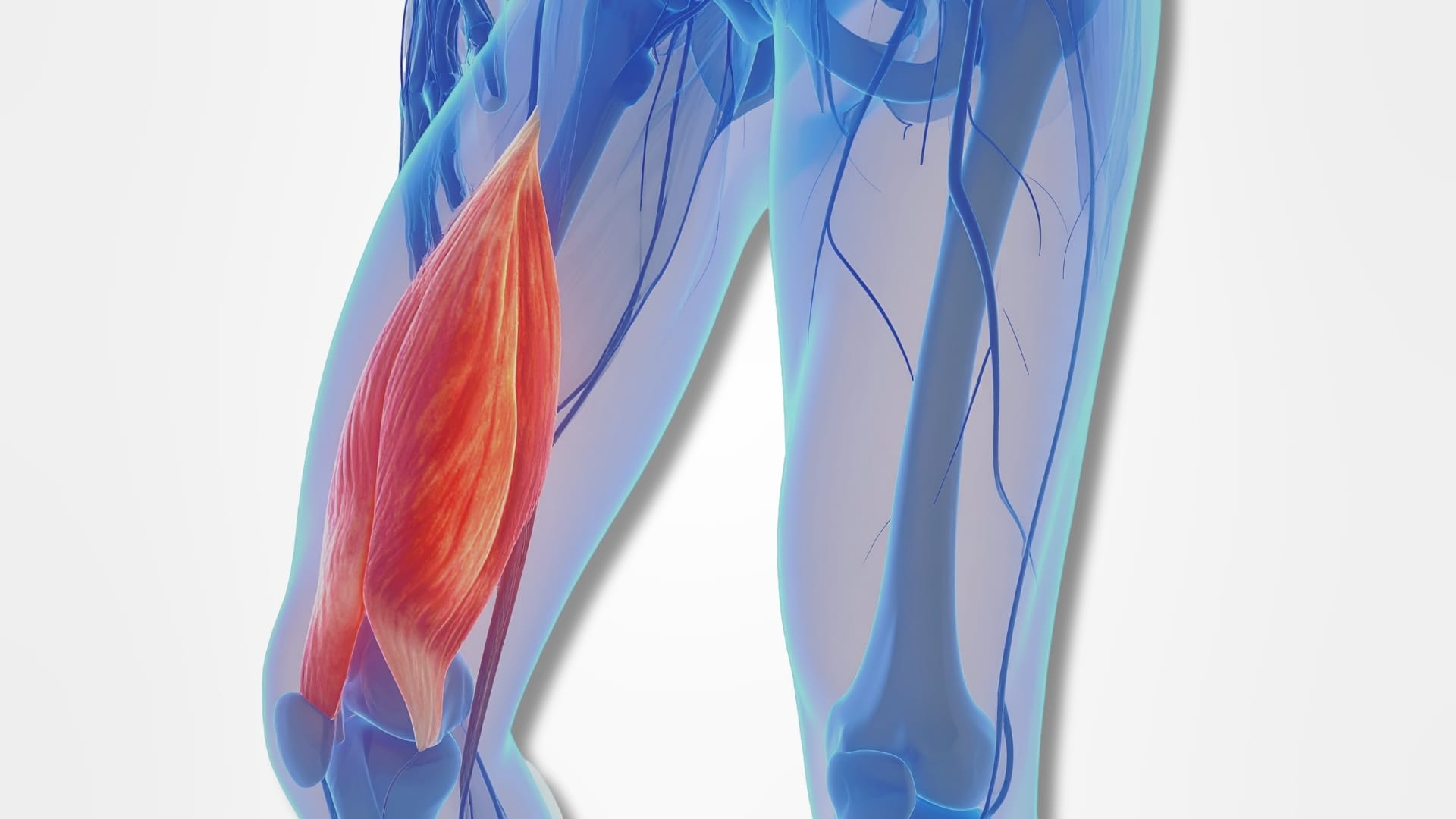
Anatomy of the Hamstring
The hamstring muscle group consists of three muscles:
- Biceps femoris
- Semitendinosus
- Semimembranosus
These muscles originate from the ischial tuberosity at the bottom of the pelvis and run down the back of the thigh, crossing both the hip and knee joints.
Their primary functions include:
- Extending the hip
- Flexing the knee
- Assisting in deceleration during running
In proximal hamstring tendinopathy, the tendon at the upper attachment point becomes irritated and degenerative due to repetitive mechanical overload.

What Is Tendinopathy?
Tendinopathy refers to a chronic tendon condition characterized by pain, impaired performance, and structural changes within the tendon. Tendinopathy is not primarily inflammatory (as the older term “tendinitis” suggests). Instead, it involves tendon degeneration due to repeated overload.
In PHT, the proximal hamstring tendon undergoes microscopic breakdown when it is stressed beyond its capacity without adequate recovery. Over time, the tendon becomes less tolerant to load, resulting in pain and dysfunction.
Causes of Proximal Hamstring Tendinopathy
Several factors contribute to the development of this condition.
1. Repetitive Overload
The most common cause is repetitive strain from activities such as:
- Long-distance running
- Sprinting
- Hill running
- Cycling
- Rowing
These activities place high tensile loads on the hamstring origin.
2. Sudden Increase in Training Volume
A rapid increase in mileage, intensity, or frequency of workouts can overwhelm the tendon’s ability to adapt.
3. Prolonged Sitting
Because the hamstring tendon attaches to the ischial tuberosity, prolonged sitting, especially on hard surfaces, can compress and irritate the tendon.
4. Muscle Imbalances and Weakness
Weak gluteal muscles or poor core control can increase strain on the hamstrings.
5. Previous Hamstring Injury
A history of hamstring strain increases the likelihood of developing tendinopathy later.

Symptoms of Proximal Hamstring Tendinopathy
Symptoms usually develop gradually and may include:
1. Deep Buttock Pain
Pain is typically localized near the sitting bone and may feel deep or aching.
2. Pain During Sitting
Sitting on hard surfaces often aggravates symptoms.
3. Pain with Running
Pain may worsen during acceleration, hill running, or prolonged activity.
4. Morning Stiffness
The tendon may feel stiff or tight upon waking.
5. Reduced Performance
Athletes may notice decreased speed, power, or endurance.
Treatment and Recovery
Managing proximal hamstring tendinopathy requires patience. Tendons adapt slowly, and recovery can take several months.
ANF Therapy®:
ANF Therapy® is an advanced approach that can be used as a complementary therapy along with traditional medical treatments in the management of hamstring tendinopathy. This therapy utilises small wearable ANF Devices that are applied to the affected areas of your body. It is totally non-invasive and chemical-free and is best for those who avoid pills and invasive procedures.
Outcomes
ANF Therapy® is a drug-free modality that has been observed in real-world clinical settings. A study involving 1,054 patients across 45 countries evaluated the use of ANF Therapy® for various musculoskeletal concerns. Commonly addressed areas included the lower back, knees, neck, and shoulders. Reported pain scores decreased from an average of 7.6 to 3.1 out of 10 following ANF Therapy® use. Participants also reported reduced swelling and improved range of motion. Overall satisfaction scores were high, while reported effects such as dry mouth, headache, or fatigue were mild and short-term.
While these findings are not specific to muscle strain alone, they reflect how ANF Therapy® can be used in supportive care settings for musculoskeletal recovery and neuromuscular balance.
Start Your Journey With ANF Therapy®
ANF Therapy® is a frequency-based approach that supports the body’s natural processes in individuals experiencing a wide range of musculoskeletal discomforts, including proximal hamstring tendinopathy. If you are dealing with ongoing muscle tension or strain in your hamstring you may consider consulting an ANF Practitioner to discuss whether ANF Therapy® could be included as part of your personal wellness or recovery strategy.
You can find an ANF Therapist by visiting: www.anftherapy.com/find-clinic.
If you are a healthcare professional interested in expanding your understanding of frequency-based approaches, you can check out more information about ANF Therapy® and the ANF Clinical Education Program at www.anfacademy.com.
Other management options include followings:
1. Load Management
The first step is modifying activities to reduce aggravating stress while maintaining general fitness.
- Reduce running volume
- Avoid hills and sprinting temporarily
- Limit prolonged sitting
Complete rest is not recommended; instead, controlled loading is essential.

2. Progressive Strengthening
Progressive loading is very important for the rehabilitation of proximal hamstring tendinopathy. Tendons require mechanical stress to adapt and become stronger, but the load must be introduced gradually and strategically. The goal is to rebuild the tendon’s tolerance to force without provoking excessive pain. This process typically moves through structured phases, each building upon the previous one.
Phase 1:
This is the starting phase. The goal is to reduce pain and gently load the tendon. Isometric exercises mean tightening the muscle without moving the joint. For proximal hamstring tendinopathy, common exercises include double-leg bridge holds and isometric hamstring curls. In a bridge hold, you lift your hips and hold the position. In a hamstring curl hold, you press your heels into the floor or a ball and hold the tension. These exercises calm pain and help the tendon handle load again.
Phase 2:
This phase begins when pain is more controlled. The goal is to build strength and make the tendon stronger. Exercises like Romanian deadlifts, hip thrusts, and Nordic hamstring exercises are used. Movements are done slowly and with control. The weight has increased gradually over time. This helps the tendon adapt safely and become more resilient.
Phase 3:
This is the final phase. The goal is to prepare the tendon for faster and more powerful movements. Tendons act like springs when running and sprinting. You start with light jogging, then move to acceleration drills, and slowly return to sprinting. This stage helps the tendon handle quick, explosive movements without pain.
What to avoid during proximal hamstring tendinopathy?
Certain treatments may not be helpful or may even delay recovery:
- Aggressive hamstring stretching (can worsen compression)
- Complete inactivity
- Repeated corticosteroid injections (may weaken tendon tissue)
Stretching into deep hip flexion can increase compression at the tendon origin and aggravate symptoms.
Recovery Timeline
Recovery varies depending on the severity and duration of symptoms.
- Mild cases: 6–8 weeks
- Moderate cases: 3–6 months
- Chronic cases: 6–12 months
Consistency in rehabilitation is more important than intensity.

How to Prevent Proximal Hamstring Tendinopathy
Once recovered, prevention is very important for maintaining tendon capacity.
- Increase training gradually (avoid sudden spikes in mileage or intensity)
- Strengthen hamstrings and glutes regularly
- Include eccentric hamstring exercises (e.g., slow lowering movements)
- Warm up properly before running or training
- Avoid prolonged sitting on hard surfaces
- Take regular breaks if you sit for long periods
- Improve running technique if needed
- Allow proper rest and recovery between sessions
- Cross-train to reduce repetitive strain
- Address muscle imbalances and core weakness
Conclusion
Proximal hamstring tendinopathy is a chronic, overuse injury that develops gradually due to repetitive stress, poor load management, or muscle imbalances. It causes deep buttock pain, stiffness, and reduced performance, particularly during running, sitting, or explosive movements. Recovery requires patience, gradual tendon loading, and structured rehabilitation to restore strength and tendon tolerance.
You can also try supportive approaches, such as ANF Therapy®, as part of a comprehensive recovery plan. Most patients feel more than50% pain reduction after the first session of ANF Therapy®. Prevention is also equally important. Gradual training progression, hamstring and glute strengthening, eccentric exercises, proper warm-ups, and avoiding prolonged sitting can help maintain tendon health and minimize the risk of recurrence.