Lower back pain is a very common musculoskeletal problem that most people experience at some point in their lives. However, one possible cause that often gets overlooked is pelvic floor dysfunction. The pelvic floor muscles help support the spine and work together with the core and lower back to keep the body stable. When these muscles aren’t working properly, it can place extra strain on the lower back, leading to pain or discomfort.
ANF Therapy® is an advanced, frequency-based approach that can be used as a complementary approach alongside standard medical treatment for musculoskeletal injuries, including pelvic floor dysfunction, under the supervision of trained ANF Therapists.
What is the role of the Pelvic Floor in Core Stability?
The pelvic floor is a group of muscles that sit at the bottom of your pelvis, forming a supportive “hammock” for the bladder, bowel, and (in women) uterus. These muscles are part of your core system, working together with:
- The diaphragm (breathing muscle)
- The transverse abdominis (deep abdominal muscle)
- The multifidus (deep spinal stabilizers)
The pelvic floor itself includes structures like the Levator Ani, which plays a major role in supporting pelvic organs and maintaining pressure control within the abdomen.
Together, these muscles create what is often called the “core canister.” If one part of this system isn’t functioning optimally, the others compensate, often leading to strain and pain.
How Pelvic Floor Dysfunction Leads to Back Pain
Pelvic floor dysfunction occurs when the muscles are:
- Too tight (overactive)
- Too weak (underactive)
- Poorly coordinated
They can contribute to back pain due to the following:
1. Tight (Hypertonic) Pelvic Floor Muscles
When pelvic floor muscles are chronically tight, they create tension in the pelvis. The pelvis and lower spine are directly connected through joints, ligaments, and muscles.
This tension can:
- Pull on the sacrum (base of the spine)
- Disrupt alignment of the pelvis
- Increase pressure in the lower back
- Irritate nearby nerves
As a result, you may feel:
- Aching in the lower back
- Tailbone pain
- Deep pelvic or hip discomfort
- Pain that worsens with sitting

2. Weak Pelvic Floor Muscles
On the other hand, weak pelvic floor muscles can not properly support your pelvis and spine. Due to this
- The lower back muscles work harder to stabilize the body
- Decrease in core stability
- Development of abnormal movement patterns
Over time, this extra strain can lead to chronic lower back pain, especially during lifting, prolonged standing, or exercise.
3. Poor Muscle Coordination
Some people experience pelvic floor dyssynergia, where muscles contract when they should relax. This poor coordination can:
- Alter posture
- Disrupt normal breathing mechanics
- Increase spinal compression
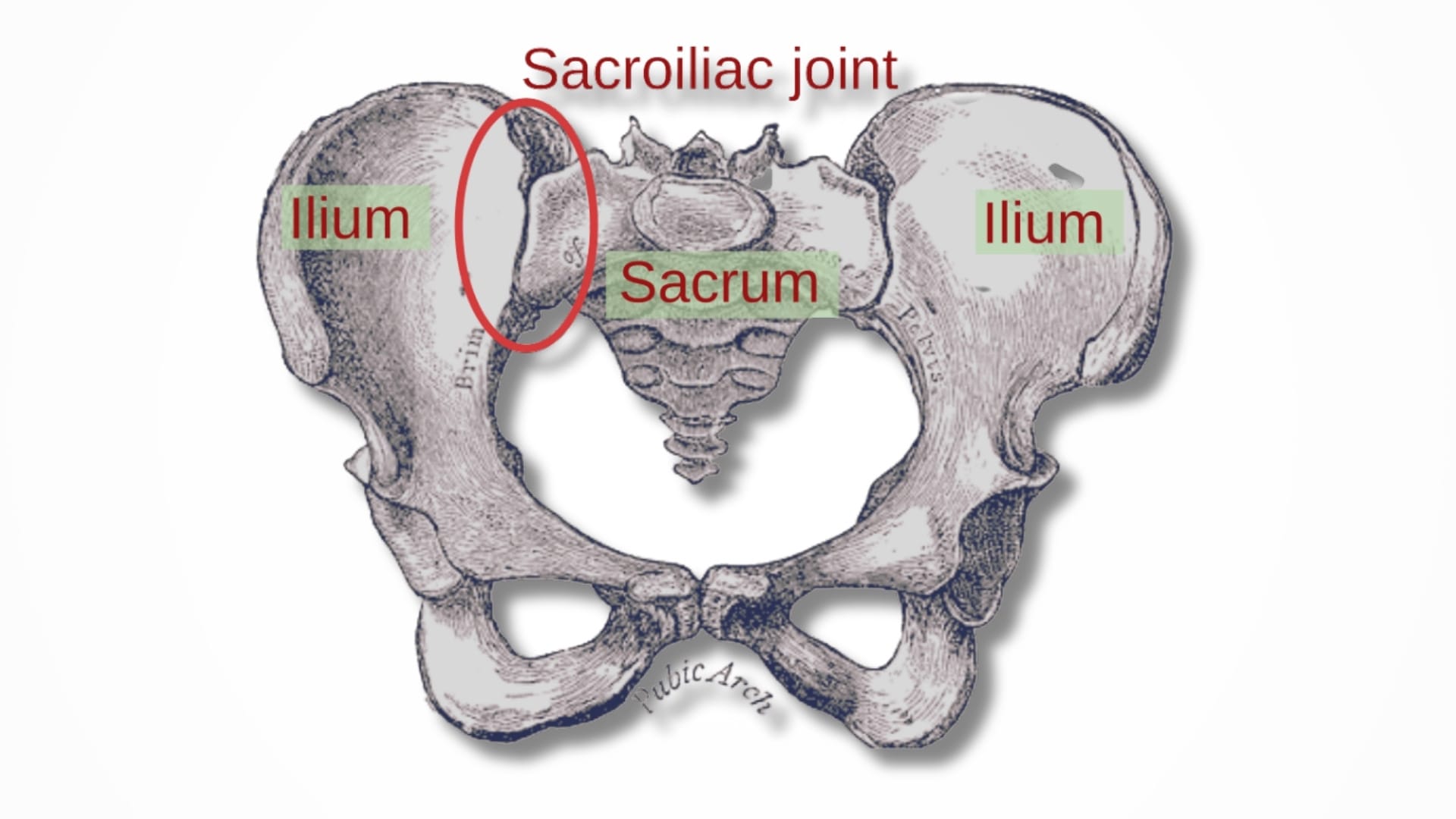
The Sacroiliac Joint Connection
The Sacroiliac Joint (SI joint) connects the sacrum (bottom of the spine) to the pelvic bones. The pelvic floor attaches in this region, so dysfunction can directly affect SI joint stability. Therefore, if pelvic floor muscles are tight or weak, they may:
- Destabilize the SI joint
- Cause inflammation
- Trigger referred pain that radiates down into the lower back, hips, or buttocks
Many people diagnosed with chronic SI joint pain later discover underlying pelvic floor dysfunction.
Symptoms of pelvic floor-related back pain
Not all back pain is related to the pelvic floor, but certain signs increase the likelihood:
- Lower back pain with urinary or bowel issues
- Pain that worsens after prolonged sitting
- Pain during or after intercourse
- Tailbone pain (coccyx pain)
- A feeling of pelvic heaviness
- Difficulty activating deep core muscles
- Back pain after childbirth
If back pain coexists with pelvic symptoms, it’s worth considering pelvic floor involvement.

Postpartum Back Pain and the Pelvic Floor
Can Men Experience This Too?
Yes, men can experience this pelvic floor-related back pain. Although pelvic floor dysfunction is more frequently discussed in women, men also have pelvic floor muscles, and dysfunction can cause:
- Lower back pain
- Groin pain
- Prostate-region discomfort
- Tailbone pain
How to manage pelvic floor-related back pain naturally?
There are multiple treatment options that can help manage pelvic floor dysfunction-associated back pain. These include followings:
1. ANF Therapy®
ANF Therapy® is an advanced, non-invasive, and chemical-free approach based on the principles of frequency medicine. It uses small, wearable devices placed on specific areas of the body to support the body’s natural regulatory and healing processes. ANF Therapy® is commonly incorporated into wider wellness and recovery programs and is applied under the guidance of trained ANF practitioners.
ANF Therapy® can complement other supportive approaches, such as physical therapy, mobility training, and strength-based exercises, to promote overall balance and recovery rather than being used as a single method.
Outcomes
ANF Therapy® is a drug-free modality that has been evaluated in real-world clinical settings. In a study involving 1,054 patients from 45 countries, the average reported pain scores decreased from 7.6 to 3.1 out of 10 after using ANF Therapy®. The most commonly supported areas included the lower back, knees, neck, and shoulders. Participants also reported reduced swelling and improved mobility. Satisfaction scores averaged 92 out of 100. Mild and short-term effects such as dry mouth, headache, and fatigue were reported by 42% of participants. These findings are encouraging, though they should be interpreted with appropriate clinical consideration.Start your journey with ANF Therapy®:
ANF Therapy® is a frequency-based approach that is used as a complementary option within wellness and recovery routines for people experiencing lower back pain associated with pelvic floor dysfunction. If you are experiencing pain and stiffness in your lower back muscles, consult an ANF Practitioner or find an ANF Therapist at www.anftherapy.com/find-clinic to discuss how ANF Therapy® can be helpful.
If you’re a healthcare practitioner and want to enhance your clinical skills with frequency medicine, learn more about the ANF Therapy® and ANF Clinical education program by visiting www.anfacademy.com.

2. Pelvic Floor Physical Therapy
Specialized therapy may include:
- Manual release of tight muscles
- Strengthening weak pelvic floor muscles
- Core stabilization exercises
- Breathing retraining
- Postural correction
Treatment is individualized based on whether muscles are tight, weak, or uncoordinated.
3. Breathing and core coordination:
Breathing and core coordination training emphasizes proper diaphragmatic breathing to support coordinated activation of the pelvic floor and deep abdominal muscles. Many people unknowingly hold their breath or brace incorrectly during movement, which can increase pressure on the spine and contribute to pain or dysfunction.

4. Stress Management
Chronic stress can lead to unconscious tightening of the pelvic floor muscles, which can increase tension and discomfort. Stress-reduction practices such as yoga, mindfulness, and relaxation techniques can help release this tension and reduce stress-related pain.
5. Posture and Ergonomic Adjustments
Improving posture and making ergonomic adjustments can significantly reduce strain on the pelvic floor and lower back. Maintaining proper sitting alignment and avoiding prolonged static positions helps support muscle balance and prevents unnecessary pressure.
Conclusion
Pelvic floor dysfunction is often overlooked as a contributor to lower back pain, yet it plays a vital role in core stability, posture, and spinal support. When the pelvic floor muscles are tight, weak, or poorly coordinated, they can disrupt the entire core system, placing excess strain on the lower back, sacroiliac joint, and surrounding structures. This can affect people of all ages and genders, including postpartum individuals and men, especially when pelvic symptoms occur alongside persistent back pain.
A comprehensive and individualized approach is essential for effective management. Supportive strategies such as pelvic floor physical therapy, breathing and core coordination training, stress management, posture correction, and complementary options like ANF Therapy® may help restore balance, reduce pain, and improve function. Addressing pelvic floor health as part of a broader musculoskeletal and wellness plan can lead to more sustainable relief and improved quality of life.
Frequently Asked Questions (FAQs)
1. Can pelvic floor dysfunction really cause back pain?
Yes. The pelvic floor is an essential part of the core system that supports the spine. When these muscles are too tight, too weak, or poorly coordinated, they can place extra strain on the lower back and sacroiliac joint, leading to pain or discomfort.
2. What does pelvic floor–related back pain feel like?
It may feel like a dull ache or persistent pain in the lower back, tailbone, hips, or pelvis. Many people notice the pain worsens with prolonged sitting, lifting, or standing, and it may be accompanied by pelvic symptoms such as urinary, bowel, or sexual discomfort.
3. Can men experience pelvic floor dysfunction and back pain?
Yes. Although pelvic floor issues are often discussed in women, men also have pelvic floor muscles. Dysfunction of these muscles can contribute to lower back, groin, and tailbone pain, as well as pelvic discomfort, in men.
4. Is pelvic floor dysfunction common after childbirth?
Yes. Pregnancy and childbirth place significant strain on the pelvic floor and core muscles. Postpartum changes can disrupt core coordination, which may lead to persistent lower back pain if not properly addressed through rehabilitation.

5. What treatments can help manage pelvic floor–related back pain?
Management may include pelvic floor physical therapy, breathing and core coordination training, stress management techniques, posture and ergonomic adjustments, and complementary approaches such as ANF Therapy®, used under the guidance of trained practitioners.6. Can ANF Therapy® be used alongside other treatments?
Yes. ANF Therapy® is commonly used as a complementary, non-invasive approach alongside physical therapy, mobility work, and strength-based exercises as part of a broader wellness and recovery program.
7. Can pelvic floor–related back pain be prevented?
Yes. Maintaining good posture, managing stress, practicing proper breathing, strengthening the core, and addressing pelvic floor issues early can help reduce the risk of developing pelvic floor–related back pain.