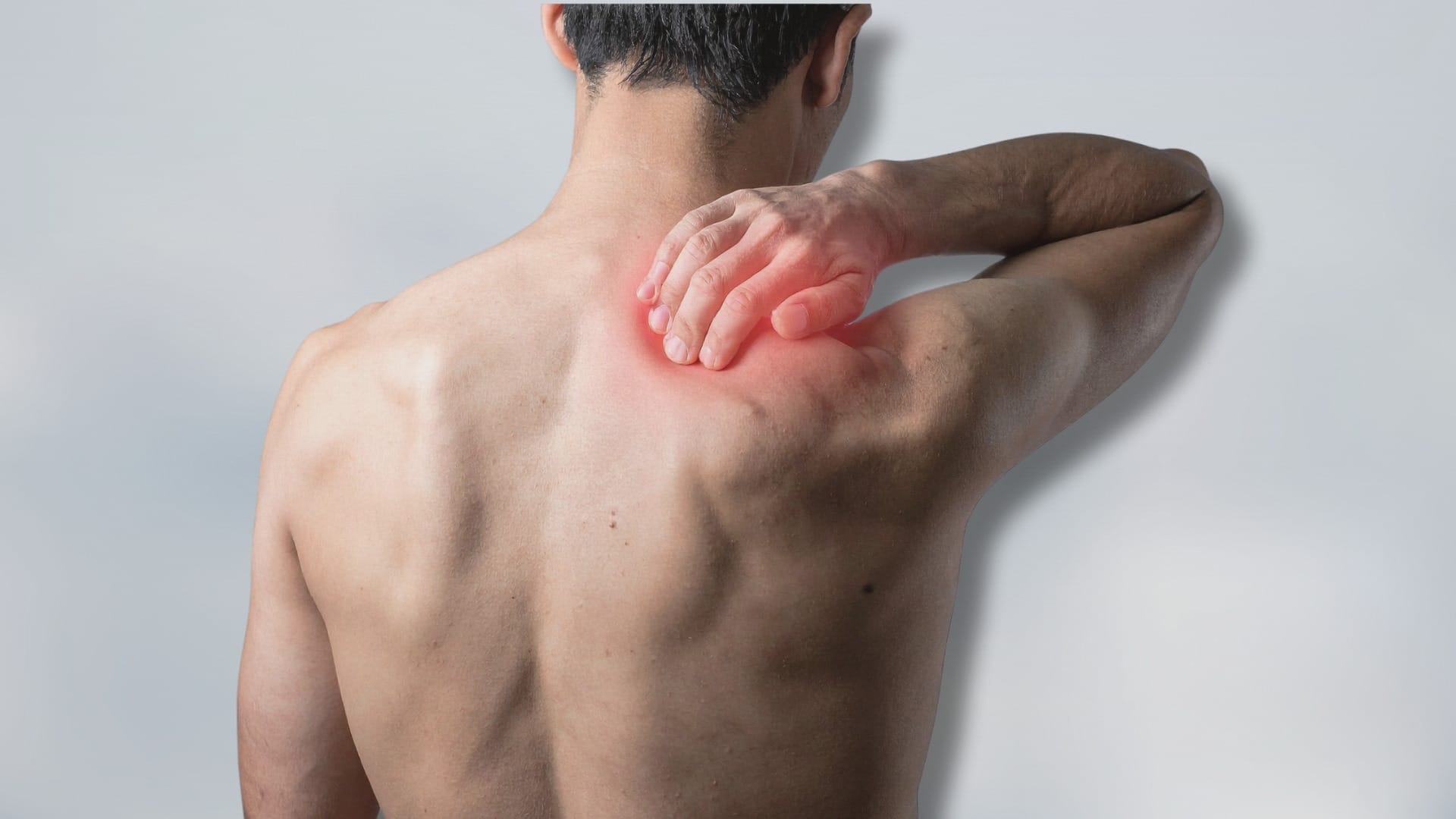
What Is Medial Collateral Ligament Bursitis?
Knee pain doesn’t just slow you down; it can make simple things like walking, bending, or climbing stairs painful. However, if you are experiencing inner knee pain, it may be due to bursitis of the medial collateral ligament (MCL). This happens when a small fluid-filled sac near the MCL becomes inflamed, leading to swelling, tenderness, and discomfort.
ANF Therapy® is an advanced complementary approach used alongside standard medical treatments to help manage MCL bursitis. It supports your overall health and wellness. In this blog, we’ll explore what medial collateral ligament bursitis is, its causes, symptoms, prevention, and how ANF Therapy® can be helpful for MCL bursitis.
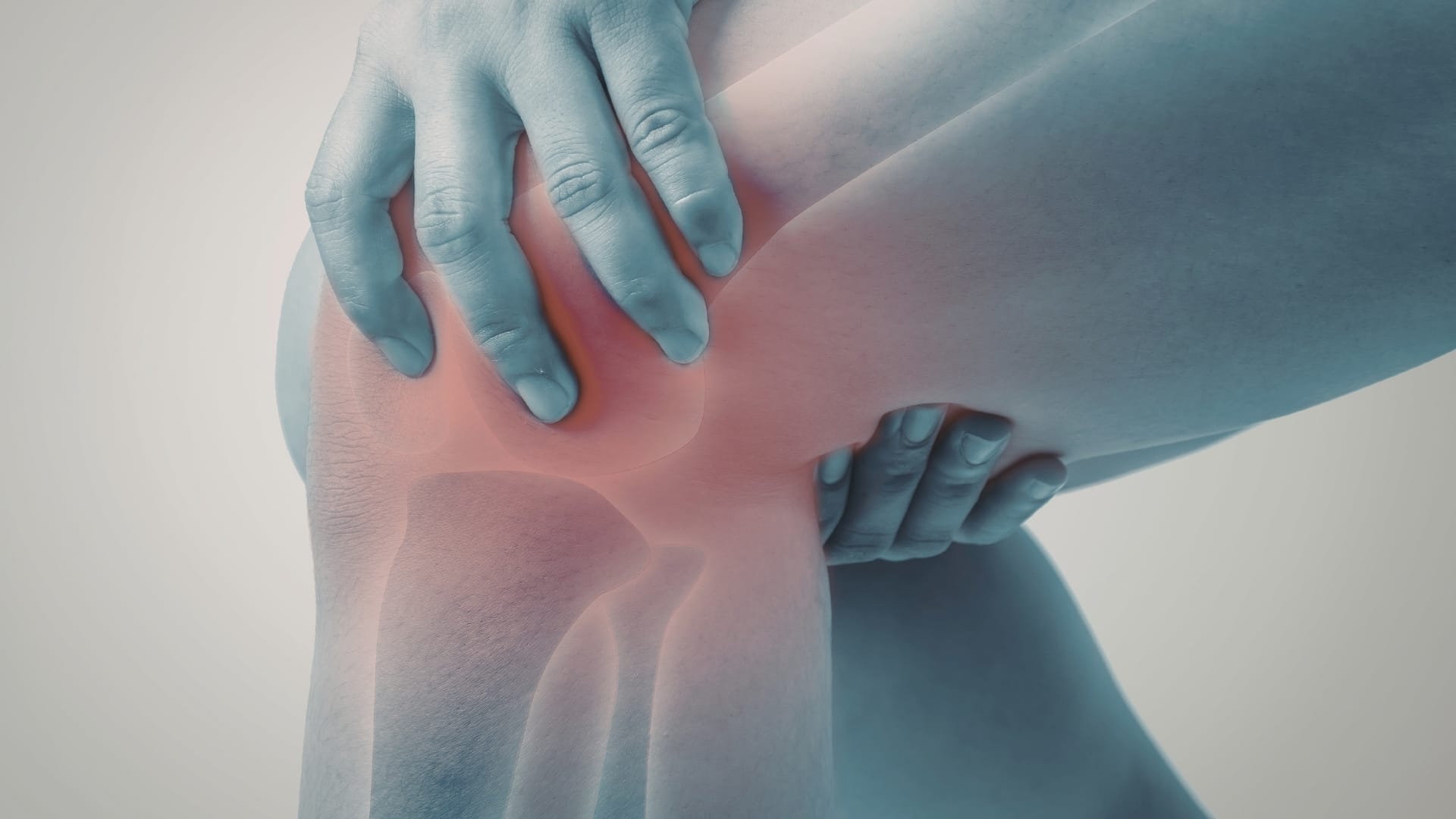
What is the Medial Collateral Ligament (MCL)
The Medial Collateral Ligament (MCL) is a strong band of connective tissue located on the inner (medial) side of the knee. It connects the femur (thigh bone) to the tibia (shin bone) and plays a crucial role in stabilizing the knee joint. MCL prevents the knee from bending inward excessively. It is particularly important during activities that involve twisting, pivoting, or side-to-side movements such as running, skiing, or contact sports.
What is a Bursa?
A bursa is a small, fluid-filled sac that acts as a cushion between bones, tendons, muscles, and ligaments. Its primary job is to reduce friction and allow smooth joint movement.
The knee contains several bursae. One of the most relevant to medial knee pain is the Pes Anserine Bursa, located on the inner side of the knee, near the MCL. When a bursa becomes inflamed, the condition is called bursitis. Therefore, medial collateral ligament bursitis refers to inflammation of the bursa near or adjacent to the MCL, causing pain and tenderness along the inner knee.

What Causes Medial Collateral Ligament Bursitis?
MCL bursitis typically develops due to irritation or repetitive stress. Some common causes include:
1. Repetitive Overuse
Activities that involve frequent knee bending, such as running, cycling, or climbing stairs, can irritate the bursa over time.
2. Direct Trauma
A blow to the inner knee (common in contact sports) can inflame the bursa and surrounding tissues.

3. Poor Biomechanics
Abnormal walking patterns, flat feet, or muscle imbalances can increase stress on the medial knee.
4. MCL Injury
A sprain or strain of the MCL may cause inflammation that spreads to nearby structures, including the bursa.
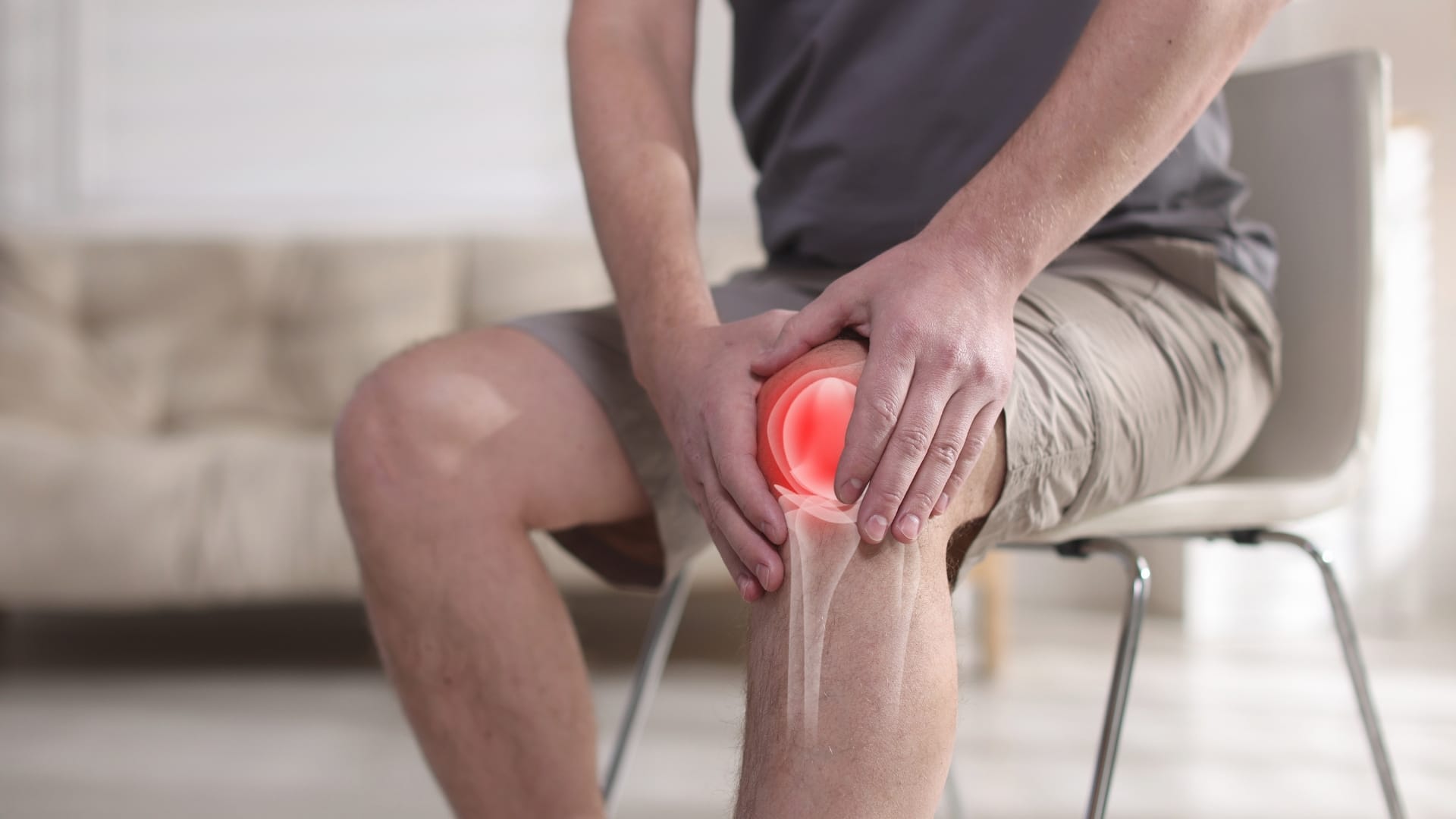
5. Osteoarthritis
Degenerative joint changes can alter knee alignment and increase friction around the medial structures.
6. Obesity
Excess body weight increases pressure on the knee joint, which can contribute to inflammation.
Symptoms of MCL Bursitis
Medial collateral ligament bursitis can cause a range of symptoms, which may develop gradually or suddenly.
Common symptoms include:
- Pain along the inner side of the knee
- Swelling or puffiness in the medial knee area
- Tenderness when pressing on the inner knee
- Warmth over the affected area
- Pain that worsens with activity
- Stiffness after prolonged sitting or inactivity
Bursitis usually does not cause significant knee instability, unlike a full MCL tear. However, discomfort can still interfere with daily activities and athletic performance.
How Is It Different from an MCL Tear?
You may confuse bursitis with an MCL injury because pain is located in a similar area.
Here’s how they differ:
| Feature | MCL Bursitis | MCL Tear |
| Cause | Inflammation of the bursa | Damage to ligament fibers |
| Swelling | Localized swelling | May include joint swelling |
| Instability | Rare | Common in moderate to severe tears |
| Pain | Achy, localized | Sharp pain after injury |
An accurate diagnosis is important because treatment strategies may vary.
How to manage the Medial Collateral Ligament (MCL)?
Most cases of medial collateral ligament (MCL) injuries and bursitis respond well to conservative treatment options.
1-ANF Therapy®:
ANF Therapy® is an advanced, holistic approach that can be used as a complementary option alongside other treatments. This method utilizes small, wearable ANF Devices that are applied to the affected areas of the body to support the body’s natural healing and regulatory processes.
Outcomes
ANF Therapy® is a drug-free modality that has been evaluated in real-world clinical settings. In a study involving 1,054 patients from 45 countries, the average reported pain scores decreased from 7.6 to 3.1 out of 10 after using ANF Therapy®. The most commonly supported areas included the lower back, knees, neck, and shoulders. Participants also reported reduced swelling and improved mobility. Satisfaction scores averaged 92 out of 100. Mild and short-term effects such as dry mouth, headache, and fatigue were reported by 42% of participants.
Start your journey with ANF Therapy®:
ANF Therapy® is a frequency-based approach that is used as a complementary option within wellness and recovery routines for people experiencing musculoskeletal issues. If you are experiencing pain, swelling, or stiffness in the inner side of your knee, consult an ANF Practitioner or find an ANF Therapist at www.anftherapy.com/find-clinic to discuss how ANF Therapy® can be helpful. If you’re a healthcare practitioner and want to enhance your clinical skills with frequency medicine, learn more about the ANF Therapy® and ANF Clinical education program by visiting www.anfacademy.com.2. Rest and Activity Modification
It is essential for recovery to reduce the activities that worsen your symptoms. Athletes or active individuals may need to temporarily avoid high-impact sports or movements that put strain on the affected area, allowing the bursa and surrounding tissues time to heal.
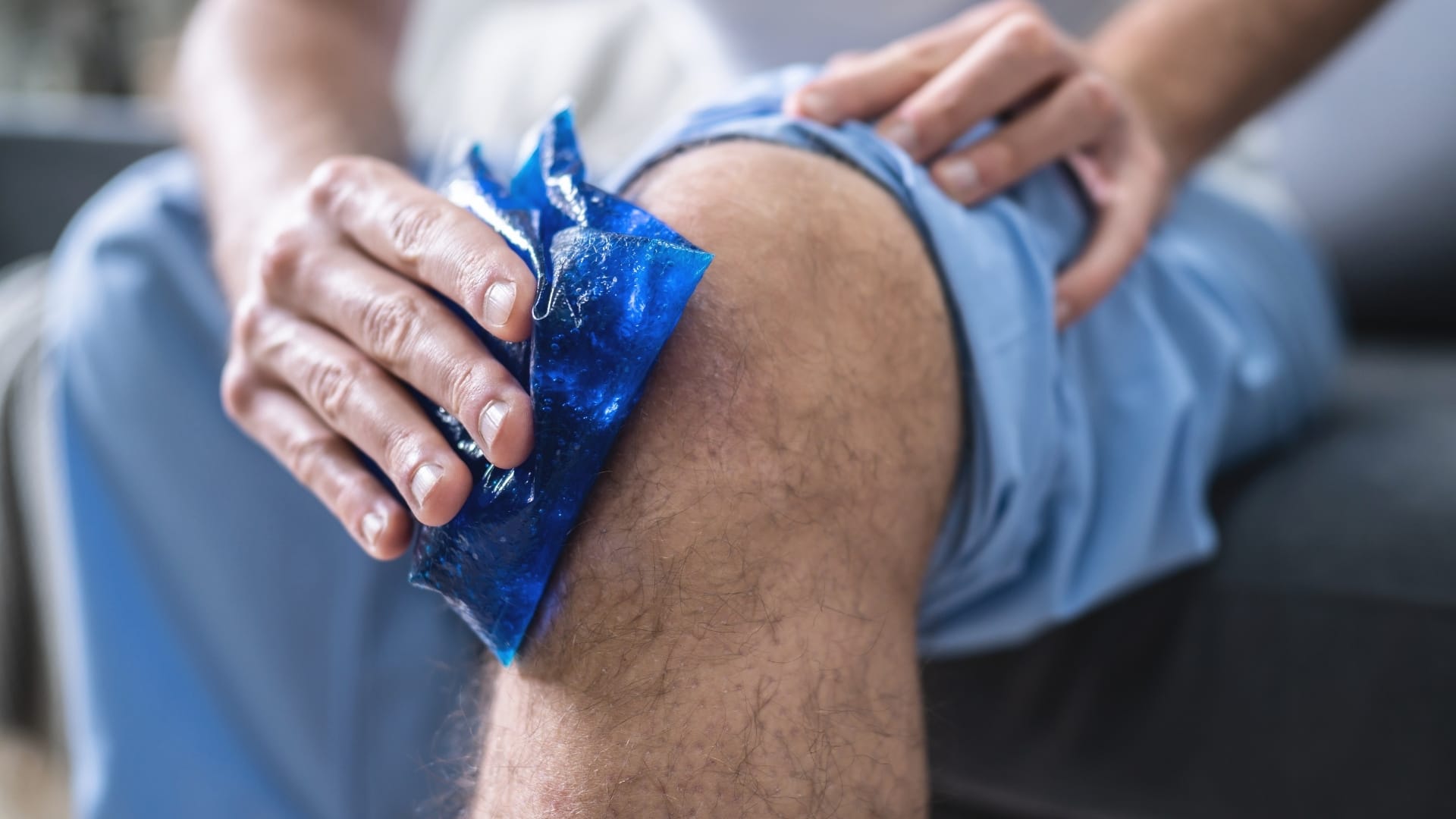
3. Ice Therapy
Applying ice for 15–20 minutes several times a day can help reduce inflammation, swelling, and discomfort. Ice therapy is particularly useful in the early stages of bursitis or after activities that aggravate symptoms.
4. Physical Therapy
A structured physical therapy program, along with ANF Therapy®, can strengthen muscles surrounding the joint, including the quadriceps, hamstrings, and hip stabilizers. Physical therapy also improves flexibility, corrects biomechanical issues, and enhances joint stability, thereby reducing the risk of recurrence.
5. Weight Management
Excess body weight can place additional stress on the knee and affected joints. Gradual weight reduction can help alleviate pressure, improve long-term outcomes, and reduce the likelihood of bursitis recurrence.
Recovery Timeline
Recovery depends on the severity of the inflammation and the timing of treatment. Mild cases may improve within a few weeks, while more persistent inflammation can take several months to fully resolve.

Can It Be Prevented?
While not all cases are preventable, you can reduce your risk by:
- Warming up before exercise
- Wearing supportive footwear
- Avoiding sudden increases in activity intensity
- Strengthening the muscles around the knee and hips
- Maintaining a healthy body weight
Conclusion
Medial collateral ligament (MCL) bursitis is a common cause of inner knee pain that can interfere with daily activities and athletic performance. It occurs when the bursa near the MCL becomes inflamed due to repetitive stress, trauma, poor biomechanics, or underlying conditions like osteoarthritis. Unlike an MCL tear, bursitis typically causes localized pain and swelling without significant instability.
Most cases respond well to conservative management, including rest, activity modification, ice therapy, physical therapy, and weight management. Complementary approaches such as ANF Therapy® can further support healing by promoting the body’s natural regulatory processes and reducing discomfort. Early recognition, proper treatment, and preventive measures such as warming up, wearing supportive footwear, and strengthening surrounding muscles can help speed recovery and reduce the risk of recurrence, allowing you to return to daily activities and sports with less pain and greater confidence.