Does Pelvic Floor Dysfunction Cause Hemorrhoids? Here’s What You Need to Know
If you have been dealing with hemorrhoids along with ongoing constipation or frequent straining during bowel movements, you might start to wonder whether something deeper is contributing to the problem. Many people ask an important question: Does pelvic floor dysfunction cause hemorrhoids?
The short answer is that pelvic floor dysfunction does not directly cause hemorrhoids, but it can significantly contribute to their development. When the pelvic floor muscles do not coordinate properly during bowel movements, the body often compensates by pushing harder. Over time, that extra pressure can lead to swelling in the veins around the rectum, which is how hemorrhoids form.
Many people focus only on treating hemorrhoids with creams, medications, or a high-fiber diet. While those approaches can help relieve symptoms, they may not address the underlying issue if pelvic floor dysfunction is involved. You need to understand how these two conditions are connected to take a more effective approach to long-term relief.
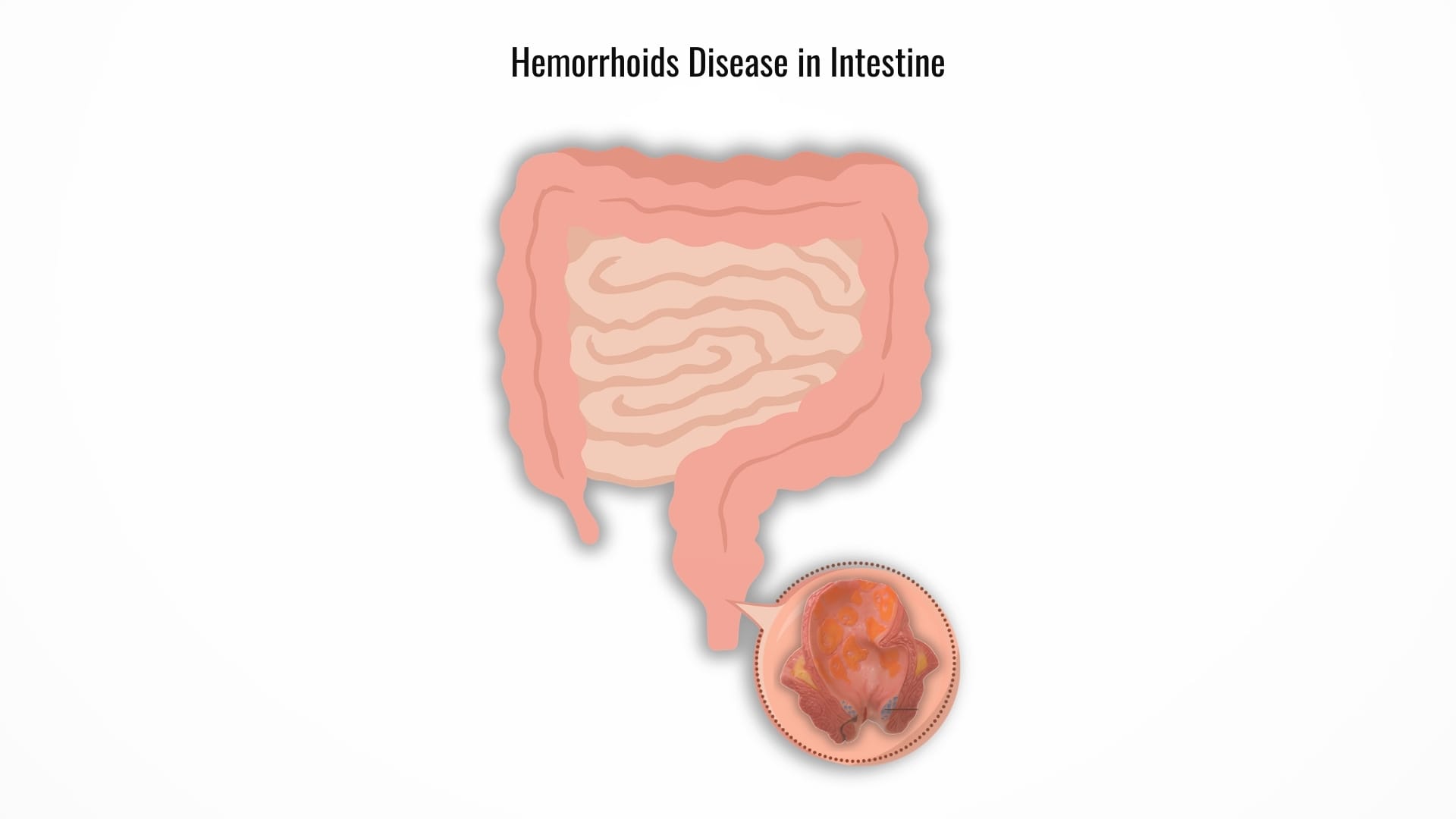
What Are Hemorrhoids?
Hemorrhoids are swollen or enlarged blood vessels located in the lower rectum or around the anus. These structures are actually a normal part of the body and play a role in maintaining continence. Problems occur when pressure in the rectal area increases, causing these veins to become enlarged and symptomatic.
People with hemorrhoids may notice several symptoms. One of the most common signs is bright red bleeding during bowel movements. You may experience itching or irritation around the anus, swelling, or a feeling of fullness in the area. External hemorrhoids can also cause pain, particularly when sitting or during bowel movements. In some cases, there may be a sensation that something is protruding from the anus.
One of the biggest contributors to hemorrhoids is increased pressure in the rectal region. Chronic straining during bowel movements is one of the most common sources of that pressure.

What Is Pelvic Floor Dysfunction?
The pelvic floor is a group of muscles located at the base of the pelvis. These muscles support several organs, including the bladder, rectum, and, in women, the uterus. They also play an important role in controlling bowel movements.
Several processes are involved in bowel movement. Abdominal pressure increases gently, the pelvic floor muscles relax, and the anal sphincter opens at the appropriate time. When these actions occur together, stool can pass without excessive effort.
Pelvic floor dysfunction occurs when this coordination does not work properly. Instead of relaxing when needed, the pelvic floor muscles may remain tight or contract at the wrong time. In some individuals, the muscles may also be weak or poorly supportive.
When the muscles do not function correctly, passing stool becomes more difficult. As a result, many people end up pushing harder than they should during bowel movements. That extra effort might not seem significant at first, but repeated straining can gradually increase pressure in the rectal veins.

How Pelvic Floor Dysfunction Contributes to Hemorrhoids
Pelvic floor dysfunction does not directly create hemorrhoids, but it can create the conditions that allow them to develop.
Chronic Straining
When the pelvic floor muscles fail to relax properly, the body naturally tries to compensate by pushing harder to pass stool. This repeated straining increases pressure in the veins of the rectum.
Over time, that pressure can cause the veins to swell. This swelling is the underlying process behind the formation of hemorrhoids. Veins are particularly sensitive to pressure, and persistent straining makes them more likely to enlarge.
Feeling Blocked or Incomplete
Many individuals with pelvic floor dysfunction describe a sensation that something is blocking the stool. This feeling often leads to a longer time spent on the toilet and repeated attempts to pass stool.
The longer a person strains, the more pressure builds in the rectal area. Multiple bathroom visits and repeated pushing can further increase congestion in the rectal veins, contributing to hemorrhoid development.
Tight Pelvic Floor Muscles
When pelvic floor muscles remain chronically tense, the pressure within the anal canal can stay higher than normal. This increased tension may affect normal circulation and contribute to venous congestion in the rectal region.
Persistent muscle tightness can make it harder for the body to regulate blood flow effectively, which may add to the conditions that allow hemorrhoids to develop.
Weak Support
In some cases, the pelvic floor muscles are weak rather than tight. When these muscles do not provide adequate support for the rectal tissues, hemorrhoids may become more prone to prolapse or bulge.
Although pelvic floor dysfunction does not directly cause hemorrhoids, it can create the pressure patterns that allow them to develop or recur.

Can Hemorrhoids Make Pelvic Floor Dysfunction Worse?
The relationship between these conditions can sometimes work in the opposite direction as well.
When hemorrhoids become painful, the body often responds by tightening the pelvic floor muscles as a protective reaction. This response is natural and is meant to guard the area from further irritation. The difficulty arises when that protective tightening does not relax afterward.
Over time, the body may develop a pattern where the pelvic floor muscles remain chronically tense. This can make it harder for the muscles to relax during bowel movements, which leads to more straining.
As a result, a cycle can develop. Pain leads to muscle tightening, which makes relaxation difficult. That difficulty leads to more strain, which can worsen hemorrhoids. Many individuals find themselves caught in this repeating loop without realizing the underlying cause.

Signs You Might Have Both Conditions
Some people may experience both pelvic floor dysfunction and hemorrhoids at the same time. Certain symptoms may suggest that pelvic floor function is contributing to the problem.
You may notice constipation that does not improve significantly with fiber intake. Excessive straining during bowel movements is another common sign. Some individuals experience a persistent feeling of blockage or incomplete emptying after using the bathroom.
Recurrent hemorrhoids can also be an indicator that pelvic floor function should be evaluated. Pain during bowel movements or the need to press around the anal area to help stool pass may also suggest coordination issues in the pelvic floor muscles.
If hemorrhoids continue to return despite dietary changes and typical treatments, it may be worthwhile to explore whether pelvic floor dysfunction is involved.

What Actually Helps?
Addressing hemorrhoids effectively often involves improving the patterns that contribute to pressure in the rectal area. The following practical strategies may help reduce strain and support healthier bowel function:
Avoid Excessive Pushing
Try not to force bowel movements. If nothing happens after a few minutes, it may be better to stand up and try again later. Remaining seated and pushing repeatedly can increase pressure in the rectal veins.
Your body typically responds better to gentle coordination rather than force. Many people find that bowel movements occur more naturally when they stop trying to push aggressively.
Adjust Your Toilet Position
Changing your toilet posture can sometimes make a noticeable difference. Elevate your feet on a small stool while sitting on the toilet to change the anorectal angle. This position may allow stool to pass more easily with less effort.

Respond to Natural Urges
When your body signals that it is time for a bowel movement, it is best not to delay. Ignoring the urge can lead to harder stool and may increase the amount of pushing required later.
Work with your body’s natural timing to make bowel movements easier and reduce unnecessary strain.
Pay Attention to Breathing
Do not hold your breath and bear down forcefully during bowel movements. A gentler approach may help. Inhale slowly and then exhale gradually while allowing the abdomen to expand. This will help your pelvic floor relax.
Consider Pelvic Floor Physical Therapy
If you suspect coordination issues, consult a pelvic health physiotherapist who can evaluate how the pelvic floor muscles are functioning. These specialists determine whether the muscles are too tight, too weak, or poorly coordinated.
They may then guide you through exercises or techniques that help retrain proper muscle function. This process often involves more than simply performing strengthening exercises, as some individuals actually need relaxation training instead.
Manage Stress
Stress can also influence pelvic floor tension. When the body remains in a prolonged state of stress, muscles throughout the body, including the pelvic floor, may stay contracted.
Practices such as diaphragmatic breathing, gentle stretching, and relaxation techniques can help normalize muscle tension and may improve bowel function.
How ANF Therapy® May Help Support Recovery
ANF Therapy® (Amino Neuro Frequency Therapy) is designed to support the body’s natural healing processes and physiological regulation. If you have pelvic floor dysfunction and hemorrhoids, ANF Therapy® may help by supporting your healing processes at the cellular level and overall wellness.
Pelvic floor dysfunction often involves altered neuromuscular signaling and autonomic imbalance. Supporting physiological regulation may complement conventional rehabilitation strategies.
It is important to understand that ANF Therapy® is not a direct treatment for hemorrhoids. Rather, it may serve as a supportive adjunct alongside physical therapy, lifestyle adjustments, and medical care.
The Bottom Line
Pelvic floor dysfunction does not directly cause hemorrhoids, but it can influence the pressure patterns that allow them to develop and recur. When the pelvic floor muscles do not coordinate properly, patients tend to push harder during bowel movements. Over time, that repeated pressure can contribute to swelling in the rectal veins.
If hemorrhoids continue to return despite changes in diet, hydration, or topical treatments, it may be helpful to look more closely at pelvic floor function. Complementary approaches may also play a role in supporting recovery. ANF Therapy® is a frequency-based approach designed to support the body’s natural processes and physiological regulation. When used alongside strategies such as pelvic floor rehabilitation, lifestyle adjustments, and appropriate medical care, it may help support neuromuscular balance and overall pelvic health.
If you are experiencing weakness or pain in the pelvis, consult an ANF Practitioner or find an ANF Therapist at www.anftherapy.com/find-clinic to discuss how ANF Therapy®can help.
If you’re a healthcare practitioner and want to enhance your clinical skills with frequency medicine, learn more about the ANF Therapy® and ANF Clinical education program by visiting www.anfacademy.com.