Most people pay attention to pelvic health only after symptoms begin interfering with daily life. A weakened pelvic floor can affect bladder control, bowel movements, posture, intimacy, and core strength. Many individuals experience symptoms for years without recognizing the root cause.
If you have ever wondered whether your pelvic floor muscles are functioning properly, this comprehensive guide will help you understand how to know if you have a weak pelvic floor, signs of weakness, risk factors, diagnostic approaches, and how you can help with it.
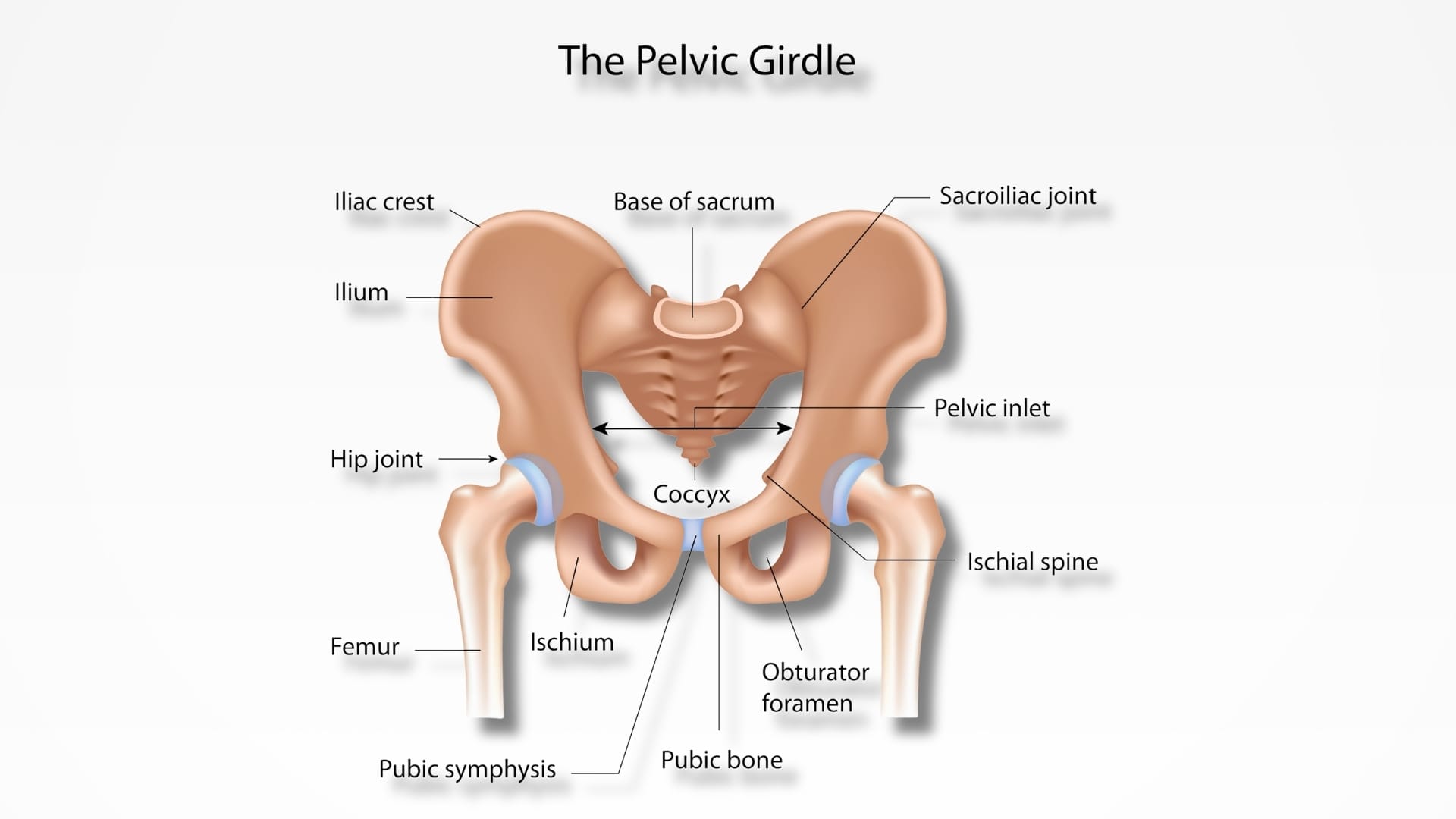
What Is the Pelvic Floor?
The pelvic floor is a group of muscles, ligaments, and connective tissues that form a supportive hammock at the base of the pelvis. These muscles support key organs, including the bladder, uterus (in women), prostate (in men), and rectum.
Functionally, the pelvic floor is responsible for:
- Maintaining urinary and bowel continence
- Supporting pelvic organs
- Contributing to sexual function
- Assisting in core stability and posture
- Coordinating with breathing and abdominal pressure
Your pelvic floor contracts when needed to prevent urine leakage and relaxes appropriately to allow urination and bowel movements. When you have pelvic floor weakness, it disrupts these movements.

What Causes a Weak Pelvic Floor?
Pelvic floor weakness develops when the muscles lose strength, endurance, or proper neuromuscular coordination. Common contributing factors of a weak pelvic floor are:
Pregnancy and Childbirth
Vaginal delivery can stretch or strain pelvic muscles and connective tissues. Women who undergo instrument-assisted vaginal deliveries and prolonged labor have an increased risk of developing weakened pelvic floor muscles.
Chronic Straining
Long-term constipation, heavy lifting, or persistent coughing due to certain diseases (such as asthma, tuberculosis, or smoking-related conditions) increases intra-abdominal pressure and weakens support structures.
Aging and Hormonal Changes
Pelvic floor muscles naturally weaken with age, especially after menopause, due to low estrogen levels. Estrogen decline affects the elasticity of connective tissue, which makes pelvic structures more vulnerable.

Obesity
Obesity significantly influences pelvic floor structure and function through mechanical loading, metabolic effects, and altered neuromuscular control. Excess abdominal fat increases intra-abdominal pressure.
This constant downward force:
- Stretches pelvic floor muscles
- Weakens connective tissue support
- Reduces muscle elasticity
- Increases risk of pelvic organ prolapse
Over time, sustained pressure leads to muscular fatigue and decreased contractile efficiency.
Pelvic Surgery
Pelvic surgery can weaken the pelvic floor muscles by disrupting the delicate network of muscles, nerves, and connective tissues that support the pelvis. During procedures such as hysterectomy, prostate surgery, or prolapse repair, tissues may be stretched, repositioned, or partially detached. These changes alter the normal functions of the muscles and reduce their ability to contract effectively.
In addition, temporary or permanent nerve irritation can impair muscle activation, while postoperative scar tissue may restrict normal movement and coordination. Pain and reduced activity during recovery can further contribute to muscle deconditioning.
High-Impact Exercise
High-impact exercise can weaken the pelvic floor when repetitive forces exceed the muscles’ capacity to absorb and counteract pressure. Activities such as running, jumping, plyometrics, and intense abdominal training repeatedly increase intra-abdominal pressure. Each forceful movement transmits downward load onto the pelvic floor. If the muscles lack sufficient strength, endurance, or coordination, repeated strain can lead to gradual stretching, fatigue, and reduced ability to contract.
Over time, inadequate recovery and poor breathing mechanics may further impair neuromuscular control, increasing the risk of urinary leakage, pelvic heaviness, or organ support issues.

How to Know If You Have a Weak Pelvic Floor?
Pelvic floor dysfunction does not develop overnight. Symptoms of a weak pelvic floor vary depending on severity. The following are a few early signs:
1. Urinary Leakage
One of the most common symptoms is stress urinary incontinence (leaking of urine) during:
- Coughing
- Sneezing
- Laughing
- Exercising
- Lifting heavy objects
If you notice leakage during physical effort, your pelvic floor muscles are not strong enough to support these movements.
2. Frequent Urge to Urinate
A weak pelvic floor can impair bladder support and coordination. You may feel urinary urgency or frequent bathroom visits.

3. Bowel Control Issues
Fecal leakage, difficulty controlling gas, or a sensation of incomplete evacuation may occur due to compromised muscular strength or weak pelvic floor muscles.
4. Pelvic Heaviness or Pressure
A dragging sensation in the lower abdomen or vaginal area may indicate pelvic organ prolapse, which can occur when the muscles supporting the organs weaken.
5. Lower Back or Pelvic Pain
The pelvic floor works with the deep abdominal muscles and diaphragm. Weakness may alter biomechanics and contribute to chronic discomfort.
6. Reduced Sexual Sensation
In some individuals, weakened pelvic muscles may affect arousal, sensation, or orgasmic intensity. If you experience reduced sexual sensation along with the above-mentioned symptoms, your pelvic floor muscles may be weak.

How to Check Pelvic Floor Muscle Weakness at Home
While a formal assessment by a pelvic health professional is the most accurate method, you can perform simple self-checks at home to identify possible pelvic floor weakness. These tests are observational and do not replace clinical evaluation, but they can help you recognize early signs.
1. The Contraction Awareness Test
Sit or lie down comfortably. Try to gently contract your pelvic floor muscles as if you are attempting to stop urine flow or prevent passing gas.
Ask yourself:
- Can you feel a lifting sensation internally?
- Are you holding your breath or tightening your glutes, thighs, or abdomen instead?
- Does the contraction feel weak or difficult to sustain?
If you cannot isolate the contraction or feel minimal lift, this may suggest weakness or poor neuromuscular control.
2. The Endurance Test
After contracting the pelvic floor:
- Hold the contraction for 5–10 seconds
- Breathe normally while holding
- Fully relax afterward
If you cannot maintain the contraction for at least 5 seconds without shaking, breath-holding, or losing intensity, endurance may be reduced.
3. The Repetition Test
Contract and relax the pelvic floor 8–10 times in a row.
Notice:
- Does strength fade quickly?
- Do contractions become weaker with repetition?
Rapid fatigue can indicate reduced muscular endurance.
4. The Functional Symptom Check
Daily-life indicators often provide stronger clues than isolated muscle testing. Consider whether you experience:
- Urine leakage when coughing, sneezing, or exercising
- Difficulty controlling gas
- Pelvic heaviness or pressure
- A sensation of incomplete bowel emptying
These functional symptoms often signal pelvic floor compromise.
5. The Mirror Observation (For Women)
Using a handheld mirror in a comfortable position, attempt a gentle pelvic floor contraction. You may observe a slight inward lift of the perineal area. If there is no visible movement or a downward bulge instead of lifting, get yourself evaluated.

Medical Diagnosis of Weak Pelvic Floor
According to the International Urogynecological Association and the American Physical Therapy Association, the diagnosis of pelvic floor muscle assessment is clinical and based on a detailed assessment.
Healthcare providers may use:
- Internal digital examination
- Biofeedback assessment
- Ultrasound imaging
- Manometry testing
A pelvic floor physical therapist is specifically trained to evaluate strength, endurance, and coordination.
Weak vs. Tight Pelvic Floor
A weak pelvic floor and a tight (overactive) pelvic floor are two distinct dysfunctions. Although both conditions affect the muscles in different ways, they can cause significant discomfort and functional problems. A weak pelvic floor occurs when the muscles lose strength, endurance, or coordination, making it difficult to support the bladder, bowel, and pelvic organs effectively. This weakness often manifests as urinary incontinence, a feeling of pelvic heaviness, fecal leakage, or even pelvic organ prolapse, where organs like the bladder or uterus descend due to insufficient muscular support.
In contrast, a tight or overactive pelvic floor refers to muscles that remain excessively contracted or hypertonic, often unable to relax when necessary. This can lead to chronic pelvic pain, difficulty urinating, constipation, painful intercourse, and a sensation of pelvic pressure. The problem here is not a lack of strength, but rather poor muscle relaxation and coordination. It is influenced by stress, trauma, postural issues, or prolonged guarding due to pain. Tight pelvic floor muscles can also create secondary problems, such as dysfunctional bowel movements or nerve irritation, because the muscles fail to lengthen and accommodate normal organ movement.
Both conditions can coexist, creating a mixed pelvic floor dysfunction, where some muscles are weak while others are overly tense. This is why assessment of pelvic floor muscles is essential. The treatment is tailored to the individual’s specific muscle patterns. Strengthening exercises may worsen tight muscles, and relaxation techniques alone may not sufficiently support weak areas.
How to Strengthen a Weak Pelvic Floor?
1. Pelvic Floor Muscle Training (Kegels)
Proper technique involves:
- Contracting as if stopping urine flow
- Holding for 5–10 seconds
- Fully relaxing between repetitions
- Repeating 8–12 times, 2–3 sets daily
Research published in journals indexed by the National Institutes of Health supports pelvic floor training as first-line therapy for stress urinary incontinence.
2. Breathing and Core Coordination
The pelvic floor functions in synergy with the diaphragm and deep abdominal muscles.
Diaphragmatic breathing improves pressure distribution within the abdomen. When you inhale, the pelvic floor gently lengthens. When you exhale, it recoils naturally. Training this coordination enhances both strength and functional control.
3. Lifestyle Adjustments
Follow these lifestyle adjustments to strengthen pelvic floor muscles:
- Maintain healthy body weight
- Avoid chronic straining
- Optimize bowel habits
- Stop smoking
- Manage chronic cough
Small daily habits significantly impact pelvic muscle integrity.
How ANF Therapy® May Help With Pelvic Floor Dysfunction
ANF Therapy® is a frequency-based approach that aims to support the body’s natural healing processes by influencing nervous system communication and tissue function. This therapy uses small, circular, and wearable ANF Devices that are applied to certain skin areas of the body.
It is important to note that ANF Therapy® is intended to support physiological processes and complement standard medical treatment rather than replacing it.
When to Seek Professional Help
Consult a pelvic health specialist if you experience:
- Persistent leakage
- Pelvic organ prolapse symptoms
- Chronic pelvic pain
- Postpartum recovery concerns
- Post-surgical pelvic issues
Early intervention prevents progression and improves long-term outcomes.
Can Weak Pelvic Floor Affect Men?

Yes. Men can experience pelvic floor weakness, particularly after prostate surgery or due to chronic straining. Symptoms may include urinary leakage, erectile difficulties, or pelvic discomfort.
Pelvic health is not exclusive to women.It is a musculoskeletal and neurological concern for all genders.
Psychological and Quality-of-Life Impact
Pelvic floor dysfunction can affect:
- Social participation
- Exercise confidence
- Sexual relationships
- Mental well-being
Because symptoms may be embarrassing, individuals often delay seeking care. However, evidence-based therapies are highly effective when appropriately applied.
Prevention Strategies for Long-Term Pelvic Health
The following are preventive strategies for improving pelvic health:
- Practicing coordinated breathing during lifting
- Avoiding chronic straining
- Strengthening deep core muscles
- Addressing constipation early
- Engaging in postpartum rehabilitation
Proactive pelvic health management is far easier than treating advanced dysfunction.
Frequently Asked Questions
Can Pelvic Floor Weakness Improve With Age?
Yes, pelvic floor weakness can improve at any age with consistent, targeted exercises. Over time, strengthening and neuromuscular retraining help restore muscle coordination and function, supporting bladder, bowel, and core stability.
Are Kegels Enough?
Kegel exercises alone may not fully address pelvic floor dysfunction. Combining them with posture correction, diaphragmatic breathing, and lifestyle modifications improves muscle coordination, reduces tension, and enhances overall pelvic support.
How Long Does It Take to See Improvement?
The timing and duration of improvement vary, but most individuals notice positive changes within 6–12 weeks of consistent, and structured training. Continued practice strengthens coordination, alleviates symptoms, and supports long-term pelvic floor function.
Final Thoughts
Pelvic floor weakness is a common but underrecognized condition that can affect bladder and bowel control, posture, core stability, and sexual function. Common symptoms of a weak pelvic floor are urinary leakage, pelvic heaviness, and reduced bowel control.
While Kegel exercises, breathing coordination, posture optimization, and lifestyle adjustments form the foundation of pelvic floor rehabilitation, integrated approaches like ANF Therapy® may provide additional support. Pelvic floor strength and function can improve at any age with early intervention, consistent practice, and a tailored rehabilitation plan.
ANF Therapy® is a frequency-based approach that is used as a complementary option within wellness and recovery routines. If you are experiencing weakness of pelvic muscles, consult an ANF Practitioner or find an ANF Therapist at www.anftherapy.com/find-clinic to discuss how ANF Therapy® can be helpful.
If you’re a healthcare practitioner and want to enhance your clinical skills with frequency medicine, learn more about the ANF Therapy® and ANF Clinical education program by visiting www.anfacademy.com.